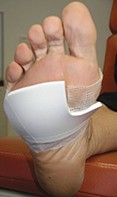
Helen’s high arch
Case history
Helen is 67 years old and has a 14-year history of type 2 diabetes that generally is well managed. She has normal foot pulses, dry but healthy skin, and clinical evidence of peripheral neuropathy with both vibration and pressure perceptions absent in the forefoot and mid foot and then reduced to the level just above the ankles.
Helen tries to walk for exercise to help blood glucose and weight control, but she often feels unstable on her feet and previously sprained both ankles when she used to play tennis. Her shoes are a slip-on, court style that show very worn down lateral heels and pressure ‘bumps’ over the toes in the shoe upper. She has a thick callus adjacent to the first metatarsal heads on both feet.
Helen says the weight bearing areas of the feet have shown callus build up in these regions for many years, but it is only in the last week that she noticed some blood on her right stocking and made an appointment to see you. She has an ulcer on her right foot surrounded by callus (Figure 1).