What’s the diagnosis?
Pruritic papules in a 10-month-old boy
Case presentation
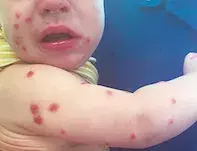
A 10-month-old boy presents with a six-week history of a pruritic eruption (Figure). He has been otherwise well, with no antecedent fevers, rhinorrhoea, cough, dyspnoea, anorexia or diarrhoea. His past medical history is otherwise normal and his immunisation record is up to date. Aside from cradle cap, he has had no other dermatological issues.
No other members of his family or any close contacts at his daycare centre have had a skin eruption of similar appearance. There is no family history of atopic dermatitis or psoriasis. His parents deny any antecedent trauma or insect bites but noticed that the onset of the rash coincided with a family holiday. They have two dogs, which live in their house.
On examination, diffusely scattered, excoriated papules and pustules are observed on the child’s face, arms, legs and trunk. He is well and interactive. There is no involvement of mucosal surfaces, dermographism or lymphadenopathy. The lesions do not urticate.
Differential diagnoses
Conditions to consider among the differential diagnoses for a child with a persistent, diffuse maculopapular and pustular eruption include the following.
- Sweet syndrome. Also known as acute febrile neutrophilic dermatosis, this idiopathic condition is characterised by peripheral neutrophilia, increased inflammatory markers (C-reactive protein [CRP], leukocytosis), fever and acute onset of a skin rash. Paediatric Sweet syndrome is rare, with fewer than 100 cases reported in the literature.1 Known associations include nonspecific respiratory or gastrointestinal tract infection, autoimmune disease (e.g. systemic lupus erythematosus), immunodeficiency (e.g. HIV infection, primary immunodeficiency), drugs (e.g. granulocyte-colony stimulating factor, all-trans retinoic acid) and malignancy (e.g. myelodysplastic syndrome, juvenile myelomonocytic leukaemia).2 Paediatric Sweet syndrome presents with acute onset of tender, erythematous papules and plaques involving the trunk and head that may appear vesiculated; mucosal involvement is rare.1,2 In addition to fever, other accompanying symptoms include conjunctivitis, arthralgia and arthritis. Visceral involvement resulting in hepatitis, pericarditis, encephalitis and myositis has been reported as extracutaneous manifestations of Sweet syndrome.2 Blood test results reflect a leukocytosis, neutrophilia and raised inflammatory markers (erythrocyte sedimentation rate [ESR], CRP). There is variability of cutaneous manifestations of paediatric Sweet syndrome, but biopsy is diagnostic and demonstrates interstitial and perivascular dermal neutrophilic infiltrate with associated leukocytoclasia and nuclear dust without fibrinoid necrosis.1
- Pityriasis lichenoides et varioliformis acuta (PLEVA). This idiopathic inflammatory dermatosis is characterised by acute onset of a maculopapular eruption at varied stages of development involving the trunk and flexural aspect of the upper and lower limbs.3 Males are slightly more affected than females. Most cases occur in the second and third decades of life, although PLEVA is also seen in paediatric populations. Despite the occasional generalised distribution of the erythematous maculopapular rash, PLEVA is usually asymptomatic, with an absence of associated constitutional signs or symptoms.3 Biopsy is diagnostic and demonstrates a diffuse and perivascular lymphocytic (CD8+ T-cells) and histiocytic dermal infiltrate with associated disruption of the dermoepidermal junction.3
- Wells syndrome. Also known as eosinophilic cellulitis, this rare idiopathic dermatosis is characterised by acute onset of erythematous bullae and plaques over 48 to 72 hours that last up to eight weeks and then spontaneously resolve.4 Constitutional signs such as fever and lymphadenopathy are uncommon.4 Associations with Wells syndrome include arthropod bites, infections, drugs (e.g. penicillin, danazol), haemoproliferative disorders and malignancy (e.g. nasopharyngeal carcinoma).4 A full blood count shows a leukocytosis and eosinophilia in half of patients, with elevated ESR and IgE levels. Biopsy demonstrates ‘flame figures’ (degenerated collagen bundles due to eosinophil major basic protein), which are indicative of, but not exclusive to, Wells syndrome.4
- Papular acral located syndrome (PALS). Also known as Gianotti-Crosti syndrome, this is a common dermatosis in the paediatric population. Associated infections are most often enteroviruses but many others have been reported, including cytomegalovirus, Epstein-Barr virus and Mycoplasma pneumoniae.5 PALS presents with an acute, symmetrical eruption consisting of monomorphic papules and vesicles favouring the extensor surfaces of the upper and lower limbs, face and buttocks that remain for approximately 10 days; there is usually sparing of the mucosal surfaces.5 Children are usually well but may exhibit a prodrome of malaise, fever, diarrhoea and lymphadenopathy. Full blood count results are variable, showing a lymphopenia or lymphocytosis.5 The diagnosis of PALS is made on a clinical basis, although biopsy demonstrates spongiosis, lymphocyte and Langerhans cell-rich vesicles, and dermal infiltrate with perivascular lymphocytes.5
- Papular urticaria. This is the correct diagnosis. Papular urticaria is a dermatosis induced by hypersensitivity to insect bites or stings.6 The pathogenesis is attributed to both immediate (initial) and delayed (late) type hypersensitivity reactions to arthropod antigens.6 Papular urticaria mostly affects children between the ages of 2 and 10 years and is responsible for approximately 5% of paediatric visits to dermatology clinics.6 Groups of erythematous, intensely pruritic papules appear on exposed areas, although the pattern of the eruption varies with the causative arthropod and can be generalised.7 The onset of papular urticaria is seasonal – it more commonly appears during the spring and summer months and is related to mosquito exposure. Household pets can harbour fleas and may be a reservoir for the ectoparasite; the presence of similar pruritic papules in other household members should raise suspicion of scabies infestation or bedbugs (Cimex lectularius).6,7 Biopsy shows dermal oedema, perivascular eosinophils, mast cells and lymphocytes.6 Papular urticaria is sometimes referred to as insect bite-induced hypersensitivity.
Diagnosis and management
The diagnosis of papular urticaria is mostly clinical and requires a targeted history to discern environmental exposures that coincided with the onset of the skin eruption. Although initial exposures to arthropods induce an immediate hypersensitivity reaction (type I), lesion persistence and/or recurrence is due to ongoing reactivation of delayed-type hypersensitivity reactions propagated by repeated exposure to arthropod antigens, which may take up to six weeks to resolve (provided that the inciting arthropod exposure is removed).6 The lesions resolve spontaneously when the child has become desensitised to the inciting arthropod antigen and/or the exposure is removed from the environment.
The treatment of papular urticaria is mostly symptom relief, with antihistamines and high-potency topical corticosteroids to treat intense pruritus. Infection control with a topical antibiotic such as mupirocin is helpful because these lesions often become superinfected as a result of scratching.
Prevention is crucial to prevent further exposure to arthropod antigens. Children should wear clothing with long sleeves and insect repellent while outdoors, particularly after dusk. Stagnant water that could encourage mosquito propagation should be removed from the garden and surrounds. Household pets should be treated for flea infestations, and household pesticide fumigation may be required for prolonged cases.
Outcome
In this patient, a skin biopsy was performed to exclude sinister diagnoses such as paediatric Sweet syndrome. A punch biopsy showed a predominantly eosinophilic cellulitis involving the dermis (superficial more so than deep). There were also scattered ‘flame figures’ to the superficial dermis. There was no evidence of vasculitis or malignancy. He commenced treatment with potent topical corticosteroids for symptomatic lesions and oral antihistamines for persistent itch, which subsequently improved. The source of the reaction was assumed to be fleas, and the family were encouraged to treat the dogs and eradicate their residence of arthropod infestation. The child’s skin eruption subsequently resolved over the following months.
References
1. Halpern J, Salim A. Pediatric sweet syndrome: case report and literature review. Pediatr Dermatol 2009; 26: 452-457.
2. Uihlein LC, Brandling-Bennett HA, Lio PA, Liang MG. Sweet syndrome in children. Pediatr Dermatol 2012; 29: 38-44.
3. Fernandes NF, Rozdeba PJ, Schwartz RA, Kihiczak G, Lambert WC. Pityriasis lichenoides et varioliformis acuta: a disease spectrum. Int J Dermatol 2010; 49: 257-261.
4. Gilliam AE, Bruckner AL, Howard RM, Lee BP, Wu S, Frieden IJ. Bullous “cellulitis” with eosinophilia: case report and review of Wells’ syndrome in childhood. Pediatrics 2005; 116: e149-155.
5. Brandt O, Abeck D, Gianotti R, Burgdorf W. Gianotti-Crosti syndrome. J Am Acad Dermatol 2006; 54: 136-145.
6. Hernandez RG, Cohen BA. Insect bite-induced hypersensitivity and the SCRATCH principles: a new approach to papular urticaria. Pediatrics 2006; 118: e189-196.
7. Demain JG. Papular urticaria and things that bite in the night. Curr Allergy Asthma Rep 2003; 3: 291-303.

