What’s the diagnosis?
A 6-month-old boy with a vesicular rash
Case presentation
A 6-month-old boy presents with a rash that has developed and evolved over the past six days. His mother says that he has been increasingly ‘clingy’ and is eating less, especially less solid food, but he has not been febrile. He has a history of atopic dermatitis, which is well controlled with topical corticosteroids.
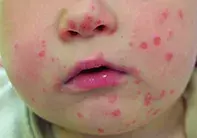
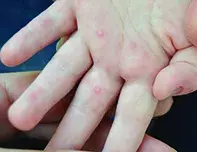
On examination, small vesicles are noted on the child’s face (Figure 1a) as well as on the soles of his feet and the palmar and dorsal surfaces of his hands (Figure 1b). His mother says that each of the vesicles initially appeared as a pink macule.
Differential diagnoses
Conditions to consider among the differential diagnoses for a child of this age include the following.
- Disseminated secondary eczema. In children, disseminated secondary eczema (‘id reaction’) is most often seen in association with tinea. The associated rash is acute, vesicular, symmetrical and extremely itchy. It is usually distributed on the limbs and face but can occur on the trunk.
- Dyshidrotic eczema. Also known as pompholyx, this condition presents as pruritic, firm vesicles and bullae on the palms and on the lateral and medial sides of the fingers. Less commonly, it can occur on the soles of the feet. Blisters are not seen anywhere else on the skin. Dyshidrotic eczema occurs mostly in patients who have a background of atopic, allergic or irritant dermatitis.
- Scabies. Scabies is a frequent cause of blisters on the hands and feet of small children and babies. It typically presents as erythematous pruritic papules, which are classically located in the interdigital webbed spaces, flexural areas of the wrists and elbows, and the feet and ankles. However, the clinical presentation of scabies is highly variable and therefore it should be considered in the differential diagnosis. In children and immunosuppressed patients, lesions can occur on the face. Vesicles and pustules can also represent scabies in children. The lesions of scabies are intensely pruritic, which was not the case in this infant.
- Bindii dermatitis. This distinctive eruption, which has been described by several Australian dermatologists, is believed to be either a foreign body reaction or an allergic reaction to the bindii seed.1 The rash presents during the spring and summer months when the spine of the bindii seed has hardened enough to penetrate the skin. An eruption of small papules or pustules occurs over the hands, knees and feet of children (usually young boys) whose skin has been pierced by the seed, most commonly when they are playing sport on a grassed area. This is not the correct diagnosis for this child, whose facial lesions were inconsistent with bindii dermatitis (and he was not mobile enough to be exposed to the seeds).
- Erythema multiforme. This acute self-limiting illness most commonly follows herpes simplex virus infection. Almost all the lesions appear in full within 24 hours. The early lesions appear as small erythematous papules that subsequently develop into the classic ‘target’ lesions. The rash most commonly appears on the face, extremities and dorsal aspects of the hands and feet but it can affect the palms and soles.
- Hand, foot and mouth disease (HFMD). This is the correct diagnosis. HFMD is the most common recognisable skin eruption caused by enteroviruses. It occurs most commonly in children under the age of 10 years, but it can affect adults and may be severe in immunocompromised and elderly people and pregnant women. The rash is characterised by small pink macules over the face and the palmar and dorsal surfaces of the hands and feet that progress to grey blisters with an erythematous halo. The red macules can also develop on the buttocks, arms and genitals. Small vesicles and ulcers also appear on the palate and in the mouth. Children are generally well but the mouth blisters can be painful and may correspond with decreased oral intake.
Investigations
HFMD is usually diagnosed clinically on the basis of the characteristic distribution of vesicles over the hands, feet and mouth. Blood tests, if performed, demonstrate raised white cell count and C-reactive protein level. PCR can be performed to detect the viral aetiology – numerous serotypes have been implicated, with coxsackievirus A16 being the most common.
Management
There are no specific treatments for HFMD. Parents should be advised that the blisters should not be ruptured and that the open wounds are contagious. Parents should be wary of the child’s oral intake if there are painful ulcers present in the mouth; in severe cases, intravenous fluids may be required.
Reference
1. Hogan PA. Bindii dermatitis. Australas J Dermatol 1997; 38: 224-225.

