What’s the diagnosis?
A pregnant woman with a pruritic eruption
Case presentation
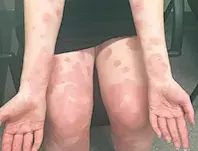
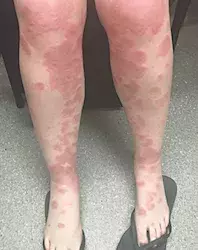
A 34-year-old woman presents at 30 weeks’ gestation in her first pregnancy with an intensely pruritic eruption (Figures 1a and b). It has been present for three weeks and is unresponsive to antihistamines. The rash started at her umbilicus and progressed to involve her trunk, arms and legs. Her face, scalp and palmar surfaces are not involved. The rash is characterised by fixed, oedematous, annular lesions that have coalesced on her trunk and limbs. Vesicles have appeared on some lesions.
The patient is otherwise well and her pregnancy is progressing normally.
Differential diagnoses
Conditions to consider among the differential diagnoses include the following.
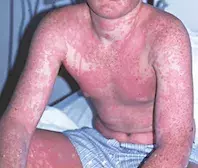
- Urticaria. This is a common IgE-mediated reaction to drugs, viruses or foods. It is characterised by pruritic evanescent oedematous wheals that ‘move’ around the body over hours. Urticaria can be quite extensive (Figure 2). It is not the correct diagnosis in this patient because her lesions are fixed and not responsive to antihistamines.
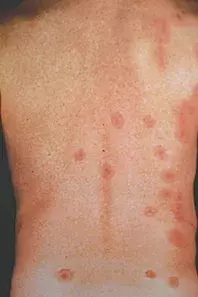
- Erythema multiforme (EM). This classic skin eruption is usually precipitated by infections, most commonly herpes simplex virus (HSV), although some drug reactions can have the same appearance. It presents with lesions that develop extensively over 24 hours. The rash is often associated with a prodrome of flu-like symptoms. The lesions may be typical or atypical targets – the former have three distinct colour zones creating a target whereas the latter are annular lesions with only two colours; both have a central vesicle (Figure 3). The lesions may have an itching or burning sensation and they can occur anywhere on the body, including the palms and soles. EM is divided into a minor form, which does not have mucosal involvement and often is a mild disease, and a major form, which has extensive mucosal involvement. EM is not the correct diagnosis in this case, as the patient had no preceding infection on history or serological investigation, there have been no new drugs, the rash does not involve the palms, and there is no mucosal involvement despite extensive cutaneous disease. In addition, the annular lesions in this patient do not have a central vesicle typical of EM.
- Polymorphic eruption of pregnancy (PEP). PEP is a relatively common pregnancy dermatosis that occurs in the last three months of gestation. It is also known as pruritic urticarial papules and plaques of pregnancy (PUPPP). The condition is thought to be an immune response to the stretching of the skin. It is characterised by red to brown pruritic papules and plaques over the abdomen, especially the striae. Atypical variants may demonstrate annular or vesicular lesions. PEP only occurs in first pregnancies. It resolves soon after delivery.
- Pemphigoid gestationis (PG). This is the correct diagnosis. PG is an uncommon dermatosis of pregnancy characterised by intensely pruritic annular and vesiculobullous lesions. It is an autoimmune condition in which IgG attacks bullous pemphigoid antigen 180 (BP180), which is located in the basement membrane. As the inflammation progresses, it causes cleavage of the epidermis from the dermis, resulting in tense vesicles and bullae. PG typically develops after 13 weeks’ gestation but can also occur in the first week postpartum. The rash is first noticed in or around the umbilicus but progresses over days to weeks to involve the trunk and limbs. The lesions are initially characterised by urticarial oedematous lesions; these lesions then develop vesicles and bullae, which are very characteristic of PG. The rash usually resolves within days of delivery but can occasionally last for many months. Relapses can occur with the return of menstruation or use of the combined oral contraceptive pill.
Diagnosis and investigations
The diagnosis of PG is made through a combination of history, examination and biopsy. Two biopsy specimens should be obtained for histology and direct immunofluorescence, which shows linear IgG and/or C3 at the basement membrane. Polymerase chain reaction testing for HSV and Mycoplasma pneumoniae is needed if biopsy results are consistent with EM.
Ongoing routine investigations and ultrasounds for the rest of the pregnancy are important because there is an increased risk of small-for-gestational-age and premature neonates.
PEP has considerable overlap for presentation with PG. However, for this patient PEP can be excluded because the rash involved the umbilicus, did not primarily involve stretch marks, and was characterised only by annular lesions.
Management
The priority of treatment is to reduce the patient’s pruritus. The rash is rarely responsive to treatment with a topical corticosteroid, and oral prednisone is almost always required at the minimum dose required to reduce symptoms. Steroid-sparing agents such as azathioprine may be needed to reduce the prednisone dose.
Secondary bacterial infection of the lesions should be treated with an oral antibiotic that has been shown to be sensitive and is safe during pregnancy. Cephalexin is Category A for use in pregnancy.
Outcome
This patient was commenced on prednisone 50 mg daily and improved rapidly. The dose was titrated down to 30 mg daily and, after the birth of a healthy infant, prednisone was withdrawn over the following two weeks without relapse.
The patient was counselled that PG would recur and would probably do so earlier in the next pregnancy. There have been cases where patients who have a subsequent pregnancy with a different partner did not experience recurrence.
Health problems in pregnancy

