It might be uncomfortable to talk about. But obesity puts children at risk of severe COVID

Vaccinating children against COVID-19 is on parents’ minds, now Australia’s rollout is open to those aged 12 and over, and regulators are actively considering vaccination for five to 11 year olds. Many parents will be thinking about the pros and cons of their children being vaccinated.
Excess weight seems to be an important factor that increases the chance of COVID-19 progressing to severe disease, including in children.
Yet the benefits of vaccines for children with excess weight or obesity hasn’t received much attention.
What does the evidence say?
Defining excess weight and obesity in a child is based on their weight and height (their body mass index or BMI). Like most aspects of health in children, that is expected to change as they grow and develop.
Many studies have shown children and young people with excess weight and obesity are more likely to go to hospital or become severely unwell with COVID-19.
A large study of more than 43,000 hospital presentations of children under 18 years in the United States showed the main background health conditions that increased the chance a child would need admission to hospital with COVID were diabetes and obesity.
If admitted to hospital with COVID, having diabetes, obesity or heart disease increased the risk of severe disease requiring intensive care.
A recent study of more than 400 COVID admissions in children from Canada, Iran and Costa Rica showed obesity was associated with severe COVID-19, particularly among those aged over 12. Obesity was the only background health condition that increased the risk (three-fold) of severe COVID-19 in this age group.

In Australia, two-thirds of children who needed ICU-level care for COVID have excess weight (weight above the 95th percentile for their age), which is at least twice the proportion of children with excess weight in the general population.
Why does weight seem to matter so much?
It is not absolutely clear, but it seems excess weight and obesity particularly affect how well our immune system can control the virus early on in the infection.
It also seems to predispose us to a poorly regulated immune response later in the infection, leading to too much inflammation.
This so-called hyper-inflammation is a key cause of severe COVID-19.
How blood vessels respond to stress and inflammation may also be compromised in people with excess weight and obesity, leading to complications such as kidney injury, blood clotting, stroke and heart attacks.
In adults, obesity is a major risk factor for severe COVID-19 too. It frequently occurs alongside diabetes, high blood pressure and other diseases in the so-called metabolic syndrome. All of these diseases have been associated with more severe COVID and similarly are linked to poorly regulated immune responses.
There may also be a mechanical effect, with obesity restricting chest wall movement reducing lung volumes and airway size under stress.
Obesity is also a leading risk factor for severe influenza, potentially through some similar mechanisms.
What can we do about it?
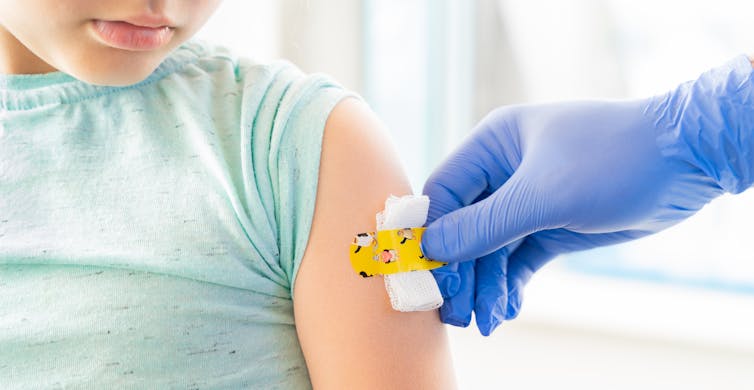
Parents need to be aware their child’s weight can affect their risk of severe COVID. These resources can help determine where your child sits in terms of their weight.
Parents should also factor their and their children’s weight into their family decisions about COVID prevention, including vaccination. If you or they are overweight, vaccines offer the best protection from COVID.
If you think your child might have excess weight, talk to your GP and consider making some changes to the family’s physical activity, screen time, sleep and eating behaviours. The Eight Health Habits fact sheet provides some starting points for families.
Obesity also needs to be factored into national decision-making around vaccination priorities. When vaccines were first made available for children aged 12-15 years, a number of health conditions were listed as “conditions associated with increased risk of severe COVID-19”. Severe obesity was on this list, but the list wasn’t ranked, so weight received very little focus.
Among all the recommended groups that should be vaccinated, people with obesity should be a top priority given it’s one of the highest risk factors for severe COVID.
Parents need to be aware of their and their children’s weight as an important issue in making decisions about vaccination.
Health practitioners and policymakers should prioritise excess weight and obesity as health conditions in current and future vaccine programs.
It might be uncomfortable to talk about, but weight is a key factor that makes COVID worse, even in children. We need to talk about it so parents can make informed decisions about their child’s risk and the benefits of vaccination.![]()
This article is republished from The Conversation under a Creative Commons license. Read the original article published on November 18, 2021.
Disclosure statement
Philip Britton receives funding from the National Health and Medical Research Council and the Commonwealth Department and NSW Ministry of Health
Louise Baur is Director of the NHMRC Centre of Research Excellence in the Early Prevention of Obesity in Childhood. She has an NHMRC Leadership Fellowship (2022-2026) which supports research in the prevention and treatment of paediatric obesity. In 2020 and 2022 she received honoraria from Novo Nordisk for educational sessions on the management of adolescent obesity (funding to her institutional research cost centre).
Nicholas Wood receives funding from the National Health and Medical Research Council for a Career Development Fellowship. He holds a Churchill Fellowship.

