What’s the diagnosis?
A child with dystrophic changes of the great toenails
Case presentation
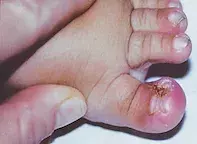
A 15-month-old boy presents with chronic recurrent dystrophy affecting the nails of both great toes since birth (Figure). His parents describe the toenails as ‘ingrown’ and have noticed more prominent erythema to the lateral hallux nailfolds over the last four months. All other nails of his feet and hands are normal.
The patient is otherwise healthy, born at 38 weeks’ gestation by normal vaginal delivery. He has met all developmental milestones to date. His immunisation record is up to date. He has a family history of psoriasis, which affects his father but does not cause nail involvement.
On examination, the great toenails of both feet show dystrophic change with lateral deviation of the nailfolds, transverse ridges, embedding and hypertrophic lateral nailfolds. No other skin, hair or other nail changes are noted.
Differential diagnoses
Conditions to consider among the differential diagnoses for dystrophic nail changes to the great toe in the paediatric population include the following.
- Onychomycosis. Onychomycosis describes a common fungal infection of the nail apparatus and is responsible for approximately 50% of nail disorder presentations.1 It is, however, unusual in children. Up to 90% of onychomycoses are caused by the dermatophytes Trichophyton rubrum and, to a lesser extent, Trichophyton mentagrophytes; the most common causative yeast is Candida albicans.1 Risk factors for onychomycosis include increasing age, diabetes mellitus, smoking and peripheral vascular disease. Onychomycoses are clinically categorised as: distal and lateral subungual onychomycosis (DLSO), superficial white onychomycosis, proximal subungual onychomycosis, candidal onychomycosis and total dystrophic onychomycosis.2 DLSO is the most common type and presents with friable dystrophic change to the lateral distal nail with associated onycholysis. Accompanying signs of tinea pedis may also be seen – that is, erythematous, macerated, scaly change to the web space between affected toes.2 Fungal scrapings taken from beneath the nail in DLSO elaborate dermatophytes or yeasts by direct microscopy; fungal culture takes at least 21 days to return a result.1,2
- Onychocryptosis. Colloquially known as an ‘ingrown toenail’, onychocryptosis is a common nail condition of the paediatric population (although uncommon in small children). Peak incidence is in the second and third decades of life, and it demonstrates a 2:1 predominance for males compared with females.3 Onychocryptosis occurs as a result of distal growth of the toenail that infringes on the nail grooves and is responsible for 20% of nail complaints to GPs.4 Risk factors include repetitive trauma, improperly fitted shoes, hyperhidrosis and distorted nail anatomy (e.g. pincer nail deformity). The condition is associated with diabetes mellitus, thyroid disease, chronic kidney and certain drugs (e.g. antivirals, ciclosporin and antifungals).4 Onychocryptosis almost always involves the hallux, with the lateral toe edges more commonly affected than the medial edges.4 It is a clinical diagnosis. Stages of onychocryptosis are correlated with severity of disease: stage I (erythema and swelling of the lateral nailfold causing pain), stage II (erythema and swelling of the lateral nailfold with associated ulceration and discharge of seropurulent material) and stage III (chronic onychocryptosis, characterised by lateral nailfold hypertrophy and granulation tissue).4
- Psoriasis. Psoriasis should always be considered among the differential diagnoses for an individual with dystrophic nail changes. Nail involvement in psoriasis is seen in 45% of individuals with cutaneous involvement and 87% of those with psoriatic arthritis.5 A small proportion of individuals (5%) will exhibit nail disease with no cutaneous or rheumatological manifestations.5 Nail psoriasis has a male predominance and is associated with larger body habitus.5 Nail changes in psoriasis can be categorised according to changes involving the nail matrix or nail bed.6 Nail pitting, which is the most common dystrophic change seen in psoriasis, leukonychia, nail plate crumbling and red spots involving the lunula are indicative of nail matrix disease.5,6 Onycholysis with surrounding erythema, oil drop discolouration, nail-bed hyperkeratosis and splinter haemorrhages are indicative of nail bed disease.5 A rheumatological assessment is indicated in an individual with psoriatic nail disease because of the known association between nail disease and psoriatic arthritis, particularly to the distal interphalangeal joints of the hands.7
- Congenital malalignment of the great toenails. This is the correct diagnosis. Congenital malalignment of the great toenails (CMGT) occurs due to lateral deviation of the nail plate with respect to the long axis of the distal phalanx of the hallux.8 The prevalence is estimated between 1 and 2% and its occurrence in families and twins (mono- and dizygotic) suggests a genetic predisposition.8,9 It is likely, however, that prevalence is underestimated, as mild CMGT may not be clinically apparent until late childhood, when activities predisposing to mechanical microtrauma (e.g. running) are more common. The pathogenesis of CMGT is unknown but potential contributory factors occurring in utero have been proposed – these include amniotic-band induced constriction of the great toes and increased intrauterine pressure – as well as unopposed tension on the lateral nailfold by the extensor tendon of the hallux.8 Unlike the other diagnoses discussed above, CMGT is present at birth but becomes more apparent as the child becomes more mobile and the toe is susceptible to repeated microtrauma. The nail changes due to CMGT include (in order of prevalence) nail plate thickening, transverse grooves, paronychia, onychocryptosis, onycholysis and a trapezoidal-shaped toenail.8 CMGT almost always involves both great toenails, with only one reported case of unilateral hallux involvement.10 Medial deviation is exceedingly rare (three cases reported).11
Diagnosis and management
CMGT is a clinical diagnosis, and adjunctive microbiological studies (i.e. bacterial swabs, fungal scrapings) are performed to assess for secondary bacterial and/or fungal infections. Management is correlated with severity of the condition. Up to 50% of cases of mild CMGT will spontaneously resolve before the age of 10 years, so a conservative approach to minimise the complications of CMGT is the initial approach (i.e. wearing properly fitted shoes to avoid onychocryptosis). Patients with severe CMGT and patients developing recurrent paronychia can be referred for surgical rotation of the nail unit, with optimal outcomes achieved when performed before 2 years of age.8
Outcome
In this patient, a clinical diagnosis of CMGT was made based on the clinical presentation and absence of cutaneous or rheumatological signs of psoriasis. Fungal scrapings taken from the hyponychium did not demonstrate fungal elements. A conservative approach was preferred by the patient’s family, and there was subsequent resolution of nail complications over the following two years.
References
1. Faergemann J, Baran R. Epidemiology, clinical presentation and diagnosis of onychomycosis. Br J Dermatol 2003; 149 Suppl 65: 1-4.
2. Roberts DT, Taylor WD, Boyle J; British Association of Dermatologists. Guidelines for treatment of onychomycosis. Br J Dermatol 2003; 148: 402-410.
3. Ikard RW. Onychocryptosis. J Am Coll Surg 1998; 187: 96-102.
4. Ezekian B, Englum BR, Gilmore BF, Kim J, Leraas HJ, Rice HE. Onychocryptosis in the pediatric patient. Clin Pediatr (Phila) 2017; 56: 109-114.
5. Tan EST, Chong W-S, Tey HL. Nail psoriasis: a review. Am J Clin Dermatol 2012; 13: 375-388.
6. Rich P, Scher RK. Nail psoriasis severity index: a useful tool for evaluation of nail psoriasis. J Am Acad Dermatol 2003; 49: 206-212.
7. Reich K. Approach to managing patients with nail psoriasis. J Eur Acad Dermatol Venereol 2009; 23 Suppl 1: 15-21.
8. Catalfo P, Musumeci ML, Lacarrubba F, Dinotta F, Micali G. Congenital malalignment of the great toenails: a review. Skin Appendage Disord 2018; 4: 230-235.
9. Chaniotakis I, Bonitsis N, Stergiopoulou C, Kiorpelidou D, Bassukas ID. Dizygotic twins with congenital malalignment of the great toenails: reappraisal of the pathogenesis. J Am Acad Dermatol 2007; 57: 711-715.
10. Batalla A, Curto JR. Congenital malalignment of the great toenail. Report of two cases. Dermatol Online J 2014; 20: 21251.
11. Baran R, Bureau H. Congenital malalignment of the big toenail: a new subtype. Arch Dermatol 1987; 123: 437.
Toe injuries and disorders

