What’s the diagnosis?
Loss of skin colour on the hands
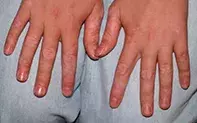
Case presentation
A 12-year-old girl presents with multiple areas of asymptomatic loss of skin colour on both of her hands that has been present for nine months (Figure). She has been otherwise well.
Differential diagnosis
Conditions to include in the differential diagnosis include the following.
- Post-inflammatory hypopigmentation. Any inflammatory process or injury (particularly a burn) involving the skin can be followed by ‘dyspigmentation’ as a result of interference in melanocyte function. Both hypo- and hyperpigmentation can occur. There is usually a history or clinical evidence of a previous traumatic or inflammatory process. In children, it commonly occurs in areas of the skin that have been affected by eczema, psoriasis or infection. There tends to be no relation between the intensity of the inflammation and the degree of hypo- or hyperpigmentation, which typically resolves without treatment over a period of months to years.
- Naevus depigmentosus (hypochromic naevus, achromic naevus). This congenital, nonprogressive disorder of skin pigmentation occurs secondary to melanocyte hypofunction and is thought to be a form of cutaneous mosaicism. It may occur as a well-defined hypopigmented patch that is present from birth or early childhood and it can become more visually apparent as the lesion grows in proportion to the child’s growth and also when the surrounding normal skin becomes increasingly pigmented (due to greater visual contrast). In some cases, naevus depigmentosus can be extensive or follow the Lines of Blaschko (embryonic cutaneous development lines) in a linear pattern. Under a Wood’s lamp (blue light), the naevus appears off-white and is no more obvious than when viewed with the naked eye. The lesions darken on exposure to sunlight because melanocytes are still present.
- Hypopigmented mycosis fungoides. Mycosis fungoides is the most common form of cutaneous T-cell lymphoma, which normally presents in adulthood and is found most often on skin in covered areas of the body rather than on the hands. The hypopigmented presentation is rare, but it is this variant of mycosis fungoides that is most likely to occur in children. The lesions can be either hypopigmented or completely depigmented macules, and there is usually some degree of epidermal irregularity – scaling or subtle wrinkling that might suggest hypopigmented eczema. It occurs more commonly in people with darker skin types, and may be completely asymptomatic or pruritic. Hypopigmented mycosis fungoides should be suspected in a patient with a hypopigmented, slightly scaly eruption that does not respond as expected to treatment. Biopsy can be helpful, but it is not always diagnostic and sometimes multiple biopsies are required. Phototherapy can be effective in treatment.
- Drug-induced hypopigmentation. This often occurs after occupational exposure to chemicals such as benzenes (hydroquinones) or acids (phenols), which have a lethal effect upon melanocytes. The hands are commonly affected, especially among workers who deal with commercial detergents and pesticides. The hypopigmentation shown in the case described above could be consistent with exposure to such chemicals, but it would be very unusual in a child.
- Vitiligo. This is the correct diagnosis. Vitiligo is characterised by ivory white macules with well-defined borders. These can vary enormously in size, from very small macules to large macules that cover extensive regions of the body. Any part of the body can be affected by vitiligo, and it is common on the dorsal surfaces of the fingers. Hypopigmented macules are usually first noted in sun-exposed regions, such as the face or hands, but areas exposed to friction and trauma are also likely to be affected.
Aetiology
Vitiligo is an acquired autoimmune depigmenting disorder in which there is genetic susceptibility. The exact aetiology is unclear, but vitiligo is thought to involve destruction of melanocytes through the action of autoreactive T-cells. The disease is common, affecting up to 1% of the population, with about half of all cases beginning in childhood. Vitiligo is gradually progressive, but there may be periods when it remains suppressed (up to years) and periods when it extends rapidly.
Investigations
Vitiligo usually has a classic appearance and does not require invasive investigations. In patients with fair skin in whom it may be difficult to differentiate between normal and affected skin, examination under a Wood’s light is an easy and noninvasive method for differentiating vitiligo from the conditions that cause skin hypopigmentation discussed above. (Under a Wood’s lamp, vitiligo-affected skin fluoresces brightly because it contains no pigmentation at all.)
Photography should be used to document disease progression. Thyroid tests and an autoimmune screen can be considered to look for disease clustering, particularly for patients who have a family history of vitiligo. Skin biopsy is rarely required but it is diagnostic, showing no melanocytes present in the epidermis.
Management
Due to the disappearance of melanocytes from the epidermis, skin affected by vitiligo has no natural sun protection. Lesions burn easily and can be complicated by skin cancer later in life. Therefore, the initial management of patients with vitiligo involves sun protection. Cosmetic camouflage is also used.
Before initiating and selecting treatment to achieve repigmentation, it is important to understand the expectations that the child and parents have regarding the condition and its prognosis, including the possibility that it may progress, and the effect that it has on the patient’s interactions with other people. Vitiligo is invariably difficult to treat, and there is no cure or known way to prevent progression. Referral to a dermatologist is recommended for a patient who wants to explore treatment options for repigmentation.
Potent topical corticosteroid or tacrolimus is considered first-line therapy for vitiligo. UVB phototherapy or psoralen with UVA phototherapy is sometimes used as an adjunctive measure. Melanocyte grafts are used in adults but are not appropriate in children.
Treatment needs to be continued for at least three months. Melanocytes often migrate from the hair follicles and reproliferate into the skin – for this reason, repigmentation is often more successful on the face and neck (where there are more hair follicles, which are the source of melanocytic repopulation of the skin) than on the hands and feet.

