What’s the diagnosis?
A nonhealing lesion on the lower leg
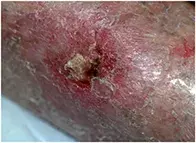

Case presentation
An 80-year-old woman presents with a painful, swollen and eroded lesion on her lower leg that has developed over four weeks (Figure 1). She has been previously well and does not recall any recent history of trauma.
The patient has a history of squamous cell carcinoma (SCC) and multiple actinic keratoses. At presentation she is well and afebrile.
A biopsy of the lesion has been performed, revealing nonspecific inflammation with no evidence of malignancy. Culture of the eroded skin overlying the lesion has returned negative results for bacteria. The patient has been prescribed two courses of cephalexin and one course of flucloxacillin, but the lesion has shown no improvement.
Differential diagnosis
Conditions to consider in the differential diagnosis include the following.
- Deep fungal infection. Fungal infection of the dermis may extend into subcutaneous tissue and bone. It is usually secondary to a penetrative injury in which deep tissue is directly inoculated with the organism. The most common deep fungal infections seen in Australia are sporotrichosis and chromoblastomycosis, which are usually found in tropical regions. The clinical appearance of these infections includes raised warty plaques, nodules (often arranged in a linear pattern known as ‘sporotrichoid spread’ due to progressive spread in dermal lymphatic vessels – see Figure 2) and ulcerated lesions. Deep fungal infections characteristically progress slowly and are most frequently located in areas that are most prone to penetrative trauma, such as the hands and lower legs, but they are uncommon in Australia. Skin scrapings are not diagnostic and confirmation is by skin biopsy, where it may be possible to visualise the organism, and tissue culture.
- Squamous cell carcinoma. An SCC should always be considered for a nonhealing ulcer – particularly in a patient who has a history of actinic damage and skin cancer. For the woman described above, her age, skin type (Fitzpatrick type 1; i.e. very fair skin, always burns and never tans) and past history place her at an increased risk of skin cancer. Widespread actinic damage in the skin surrounding the lesion, characterised by solar elastosis, hyperkeratosis and irregular pigmentation, is suggestive of chronic sun exposure. The lower limb is a common location for skin cancer, especially in women. The characteristic SCC is inflammatory with erythema and hyperkeratosis, and is firm and scaly. As it progresses there may be ulcer development. However, an SCC tends to be relatively slow growing, and the history of this woman’s lesion, which appeared over about four weeks, would be unusual for an SCC. A skin biopsy would confirm the diagnosis.
- Cellulitis. A patient with this localised bacterial infection of the skin, which is most often caused by Staphylococcus aureus or Group A streptococcus, would typically have additional features, including more prominent swelling and erythema and localised warmth. Lower leg cellulitis is usually accompanied by fever, malaise, pain and lymphadenopathy. Although the response to oral antibiotics may be slow in elderly patients, particularly if they do not rest, it would be very unusual for cellulitis to be completely unresponsive to treatment unless it involved a resistant organism (which would be evident on culture).
- Atypical mycobacterium infection. This is the correct diagnosis. It refers to infection with any mycobacterium other than Mycobacterium tuberculosis, which is responsible for pulmonary and cutaneous tuberculosis. In Australia, the most common causes of atypical mycobacterium infection are Mycobacterium ulcerans and Mycobacterium marinum. Atypical mycobacteria are usually acquired from water or soil, and it is likely that this patient was exposed on the farm where she lives. There is sometimes no history of obvious trauma, as in this case, and there may be a lag of several weeks between inoculation and evidence of infection. In a patient with dry, sun-damaged skin the organism could enter through a small fissure. The typical lesion begins as a subcutaneous nodule that may progress to develop pain, swelling and ulceration, as occurred in this case. In other cases the lesion appears as a nonspecific granuloma.
Investigation and diagnosis
The most common cutaneous infective bacterial agent causing chronic infection is Staphylococcus aureus. For a patient with a nonhealing lesion that has not responded to antistaphylococcal antibiotics, a biopsy should always be performed to rule out malignancy. Once malignancy has been excluded, fresh tissue should be sent for culture and polymerase chain reaction (PCR) analysis, with the laboratory informed of clinical suspicion of atypical mycobacterium infection so that the specimen can be set up on specific media to identify the organism. Despite this, however, culture and PCR are often unsuccessful in identifying atypical mycobacteria. Histology of tissue may show only nonspecific changes with lymphohistiocytic infiltrate and scattered neutrophils. The presence of a granulomatous infiltrate is very suggestive in this clinical setting.
Management
Some atypical mycobacteria are very slow growing in the laboratory and it is often a number of weeks before the result of culture is known. However, this should not delay treatment. This patient was treated empirically with minocycline, 100 mg daily for 12 weeks, which resulted in healing of the lesion. The specimen of tissue cultured did not ultimately identify an organism and the presumptive diagnosis of atypical mycobacterium infection was made on the basis on her response to treatment. Ideally, the antibiotic of choice is determined by isolation of the causative organism and sensitivities, but a scenario where the laboratory results are not available is not uncommon in atypical mycobacterium infection and a clinical decision regarding treatment has to be made. Ciprofloxacin and clarithromycin are also effective but incur greater cost to the patient. Antibiotics usually need to be taken for a prolonged period to achieve resolution of atypical mycobacterium infections.

