What’s the diagnosis?
Sudden onset of blisters on the arms and neck
Case history
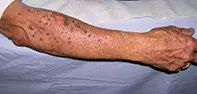
A previously well, 56-year-old woman presents with sudden onset of a bilaterally symmetrical blistering eruption on her neck and forearms (Figure 1). The rash does not involve any other part of her skin and her face is spared.
The itchy blisters developed the day after the patient spent a day in the garden. She had worn a short-sleeved, V-neck shirt, gardening gloves and a broad brimmed hat, and she had applied a sunscreen that she had used many times before but mainly to her face. Three weeks ago she had commenced treatment with diltiazem. Her other medications, simvastatin, paracetamol and vitamin D, are longstanding.
Bacterial swabs of the lesions do not show any pathogens.
What is the most likely cause of this rash? What would you consider in the differential diagnosis?
Diagnosis
The patient was diagnosed with a photosensitive drug eruption, a rash that is found only in areas that are exposed to ultraviolet light. These eruptions can have an unpredictable distribution because not all areas are equally exposed to ultraviolet light and patients often apply more sunscreen to their faces than to other parts of the body. It is not uncommon to find blisters, which may or may not occur on an erythematous background.
Diltiazem is known to cause a photosensitive drug eruption but it is not common, occurring in less than 1% of patients taking this drug. This patient was not sufficiently sun-exposed to induce a reaction for the first three weeks of diltiazem therapy, but as soon as she spent a day gardening the rash appeared.
Differential diagnosis
Conditions that should be included in the differential diagnosis include the following.
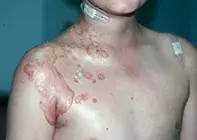
- Bullous impetigo, which is caused by Staphylococcus aureus (Figure 2). This is not usually bilaterally symmetrical. However, it is often of sudden onset and, on probability, acute bullous impetigo is much more likely than a drug reaction for the patient described above. However, swabs of the lesions would be expected to demonstrate the organism.
- Photoallergic contact dermatitis to an applied medication can cause diagnostic confusion. Ironically, one of the most common causes is sunscreen itself. However, a reaction like this would be expected to be confluent rather than to consist of discrete lesions, although blisters may occur in all patients with contact dermatitis. This patient has been using the same sunscreen previously without problems, making this an unlikely cause.
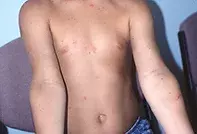
- Allergic contact dermatitis to plants and to airborne substances should be considered, particularly for a patient who has spent time in a garden. Plant dermatitis usually presents with blistered streaks where a plant has brushed against the skin (Figure 3). It may appear to have a sun-exposed distribution, but it actually occurs on areas of bare skin that have contact with the plant. Airborne substances such as pollens usually produce a confluent erythematous reaction rather than blisters.
- Immunobullous diseases, such as bullous pemphigoid and pemphigus, are rare and not usually photo-distributed. They are, however, more common in middle-aged and elderly women.
- Lupus erythematosus should be considered in any rash that has a photo-distribution. Blistering may occur, but this is unusual.
- Porphyria cutanea tarda is another rare skin disease that may cause a blistering rash on light-exposed areas. Patients are genetically predisposed by lack of a hepatic enzyme (uroporphyrinogen decarboxylase) and are often alcohol dependent. Blistering usually occurs only on the dorsa of the hands and forearms. It is associated with dyspigmentation and scarring.
Clinical spectrum
Most photosensitive reactions are phototoxic (nonimmune) rather than photoallergic. Patients initially complain of a burning sensation on light-exposed areas, followed by erythema, oedema and sometimes blistering. The distribution of the rash can be puzzling because not all light-exposed areas are involved.
Drugs that may be implicated in photosensitive drug reactions include NSAIDs such as ibuprofen, as well as sulfa and tetracycline antibiotics, thiazide diuretics, amiodarone and other anti-arrhythmic agents and antihypertensive agents.
Investigation
A skin biopsy submitted for plain and immunofluorescent microscopy will rule out immunobullous disease and lupus erythematosus, and a swab will rule out bullous impetigo. Skin biopsy in drug reactions is not always diagnostic.
The distribution of the rash on light-exposed areas and the recent introduction of a known phototoxic agent are suggestive of the diagnosis. Phototesting may be carried out at specialty patch test clinics. To access these, patients should be referred to a dermatologist.
Management
The simplest and most effective treatment for a photosensitive drug eruption is simply to stop the drug and replace it with an alternative that is not phototoxic. For patients taking amiodarone this may be difficult – in this situation, a reduction in drug dosage (if possible) together with sun avoidance and use of a broad-spectrum sunscreen will assist.
Drug reactions

