What’s the diagnosis?
A child with sudden onset of dry, hyperpigmented skin
Case presentation
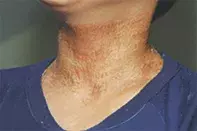
A 10-year-old boy presents with a painless, nonpruritic eruption affecting his neck (Figure). The skin is dry and hyperpigmented. The eruption appeared suddenly during a flare of eczema that is being treated with topical corticosteroid, emollient and a bath oil containing the antiseptic triclosan.
Differential diagnoses
Conditions to consider among the differential diagnoses include the following.
- Contact dermatitis. Sensitisation to triclosan can occur but is rare. In a study of 275 participants with chronic eczema, only two patients (0.7%) developed positive reactions to triclosan and four patients (1.4%) to triclosan-based products.1 Contact dermatitis is erythematous, oedematous and pruritic – this child presented without these signs or symptoms so other diagnoses should be considered.
- Eczema flare. Flares of eczema are typically accompanied by signs of erythema and fresh excoriations, and symptoms of pruritus and soreness. Hyperpigmentation is not a feature.
- Chemical burn. This is the correct diagnosis. Chemical burns typically present as erythema, rapidly followed by hyperpigmentation and exfoliation. If they are mild, as in this case, they are painless. Topical triclosan, an antiseptic, has been known since the 1990s to be effective for atopic dermatitis owing to its antimicrobial, antifungal and anti-inflammatory properties.2 More recently, however, it has been found that triclosan-containing products can interact with chlorine (in tap water) to form chloroform,3 which has been deemed by the United States Environmental Protection Agency a probable human carcinogen.4 Triclosan is a precursor of dioxins, which can harm the human endocrine system and the environment. Under certain conditions, triclosan may increase an individual’s overall annual exposure to chloroform by 15% to 40% above background tap-water levels.5 Exposure to triclosan and its by-products such as chloroform can result in a chemical burn, as this patient suffered.
Diagnosis
The diagnosis of a chemical burn resulting from triclosan treatment can be made on the basis of the patient’s history and the classical clinical findings.
Management
Management of a chemical burn caused by triclosan requires avoiding re-exposure to the causative ingredient.
This patient ceased using the triclosan-containing bath oil and commenced a topical emollient. His skin returned to normal in two weeks and the hyperpigmented areas peeled off. His parents were advised to use plain chlorine bleach in the bath in future if an antiseptic is required during eczema flares, as this is a much safer alternative.6
References
1. Schena D, Papagrigoraki A, Girolomoni G. Sensitizing potential of triclosan and triclosan-based skin care products in patients with chronic eczema. Dermatol Ther 2008; 21 Suppl 2: S35-S38.
2. Sporik R, Kemp AS. Topical triclosan treatment of atopic dermatitis. J Allergy Clin Immunol 1997; 99: 861.
3. Levin C, Warshaw E. Triclosan: an update on safety. Dermatitis 2007; 18: 234-235.
4. United States Environmental Protection Agency. Chloroform. Available online at: www.epa.gov/sites/production/files/2016-09/documents/chloroform.pdf (accessed May 2019).
5. Campbell L, Zirwas MJ. Triclosan. Dermatitis 2006; 17: 204-207.
6. The Royal Children's Hospital Melbourne. Formula for an eczema bath. Available online at: www.rch.org.au/uploadedFiles/Main/Content/derm/eczema-bath-information.pdf (accessed May 2019).
Drug reactions

