Peer Reviewed
Feature Article Infectious diseases
Herpes simplex virus and varicella zoster virus infections: clinical presentations and treatment strategies
Abstract
The ability of herpes viruses to establish latency enables them potentially to cause clinically significant disease in the future. Management strategies are thus aimed at reducing virus transmission and patient morbidity.
Key Points
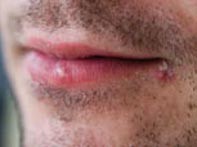
- Herpes simplex viruses 1 and 2 (HSV-1 and HSV-2) can cause both primary and recurrent symptomatic or asymptomatic infections, mainly involving the orolabial and genital areas.
- Diagnosis of clinical HSV infection requires virus identification from specimens, usually swabs taken from herpetic lesions. Nucleic acid tests are the most sensitive methods available.
- Counselling and patient education are essential in the management of patients with genital herpes.
- Oral antiviral treatment is indicated for severe nongenital herpes and for initial genital herpes. Patients with frequent recurrences of HSV infection may require continuous antiviral therapy (suppressive therapy) or intermittent antiviral therapy (short-course episodic therapy) that is instituted with the onset of symptoms.
- The primary varicella zoster virus (VZV) infection varicella (chickenpox) and the reactivated infection herpes zoster (shingles) are usually diagnosed clinically.
- Diagnostic modalities available for VZV infection are similar to those used for detection of HSV infection.
- Antiviral therapy is indicated in herpes zoster within 72 hours of onset for all patients over 50 years, to reduce the risk of developing postherpetic neuralgia.
Purchase the PDF version of this article
Already a subscriber? Login here.