What’s the diagnosis?
A baby with a raised brown lesion on the leg
Case presentation
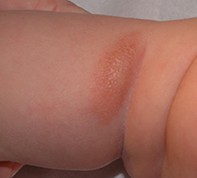
A 9-month-old girl presents with a single plaque (3 x 1 cm) located over the posterior aspect of the knee (Figure). The lesion, which is raised and light brown in colour, first appeared when she was three months of age. At first the lesion blistered recurrently, and it was treated with topical mupirocin several times. The blistering stopped after three months, but the lesion has persisted. Her parents have noted that from time to time the lesion swells and becomes erythematous, returning to normal over about 20 minutes.
Differential diagnosis
Conditions to include in the differential diagnosis for a child of this age include the following.
- Congenital melanocytic naevus. This lesion is usually very well defined and it has a characteristic appearance under dermoscopy. It is unusual for melanocytic naevi to first appear in the first year of life; larger ones are usually present at birth. They do not blister.
- Spitz naevus. This benign melanocytic lesion occurs most commonly in the paediatric population. It often presents as a round, firm, papular or nodular lesion with a red-brown colour. A Spitz naevus may be completely amelanotic and cannot always be diagnosed by dermoscopy. It usually has a rapid period of growth before becoming static. Being a melanocytic lesion, it does not blister.1
- Juvenile xanthogranuloma. This is an uncommon benign histiocytic tumour of infancy and early childhood. It has a characteristic appearance on biopsy and on dermoscopy appears yellow and amorphous. These lesions appear rapidly and vary in size from a few millimetres to several centimetres. They do not swell when rubbed and they do not blister. They typically resolve spontaneously and therefore do not require treatment.2
- Insect bite. Itch, redness and blistering could be expected from an insect bite. However, such lesions do not persist for months. They are erythematous rather than light brown in colour.
- Bullous impetigo. This skin infection is characterised by superficial blisters that rupture and crust. However, impetigo does not present as a persistent raised lesion. Bullous impetigo responds to mupirocin and a swab of the lesion will test positive for Staphylococcus aureus.
- Mastocytoma. This is the correct diagnosis. A mastocytoma is a solitary lesion that occurs most commonly in young children and rarely in adults. Blistering may occur initially, especially in areas that are susceptible to friction, such as the nappy region, but usually stops within a few months.
Clinical features
A mastocytoma is usually a spot diagnosis. A positive Darier’s sign (swelling and increase in erythema of the lesion in response to stroking or rubbing) is highly suggestive of the diagnosis, although not pathognomonic.3 Symptomatic flushing can occur as a result of histamine release.
Dermoscopy is nonspecific in mastocytoma. In some cases, a biopsy is required to confirm the diagnosis; this will reveal infiltration of mast cells through the upper dermis or the full thickness of the skin.4
A mastocytoma is a benign solitary lesion. However, multiple lesions may occur in an uncommon condition called mastocytosis, in which there is an excess collection of mast cells that release vasoactive chemical mediators, including histamine.5 Disorders relating to mastocytosis can be limited to the skin or systemic.6
Management
A child presenting with a solitary mastocytoma does not usually require specific treatment. Parents should be reassured that the lesions are benign and usually involute over the first few years of childhood. Treatment is directed at symptomatic relief – flushing and pruritis can be treated with an antihistamine and potent topical corticosteroid.7
Further investigation is warranted if systemic mastocytosis is suspected in a child with a history of diarrhoea and wheezing. In this situation, referral to a dermatologist is recommended. Simple flushing is not considered a cause for concern. A serum tryptase measurement will give an indication of mast cell load; it would be very unusual for this be elevated in a patient with a solitary mastocytoma.
References
1. Barnhill RL. The spitzoid lesion: rethinking Spitz tumors, atypical variants, ‘Spitzoid melanoma’ and risk assessment. Mod Pathol 2006; 19 Suppl 2: S21-S33.
2. Janssen D, Harms D. Juvenile xanthogranuloma in childhood and adolescence: a clinicopathologic study of 129 patients from the Kiel Pediatric Tumor Registry. Am J Surg Pathol 2005; 29: 21-28.
3. Soter NA. Mastocytosis and the skin. Hematol Oncol Clin North Am 2000; 14: 537-555.
4. Horny HP, Metcalfe DD, Bennett JM, et al. Mastocytosis. In: Swerdlow SH, Campo E, Harris NL, et al (eds). WHO Classification of tumours of haematopoietic and lymphoid tissues. 4th ed. Lyon, France: WHO; 2008. pp 54-63.
5. Hartmann K, Henz BM. Mastocytosis: recent advances in defining the disease. Br J Dermatol 2001; 144: 682-695.
6. Valent P, Sperr WR, Schwartz LB, Horny HP. Diagnosis and classification of mast cell proliferative disorders: delineation from immunologic diseases and non-mast cell hematopoietic neoplasms. J Allergy Clin Immunol 2004; 114: 3-11.
7. Barton J, Lavker RM, Schechter NM, Lazarus GS. Treatment of urticaria pigmentosa with corticosteroids. Arch Dermatol 1985; 121: 1516-1523.
Skin lesions

