What’s the diagnosis?
A boy with a purpuric rash of sudden onset
Case presentation
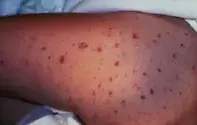
A 10-year-old boy presents to the emergency department of his local hospital with a purpuric rash of sudden onset on his buttocks and legs (Figures 1a and b). He has a fever and headache.
Differential diagnosis
Conditions to include in the differential diagnosis for a child of this age include the following.
- Leukocytoclastic vasculitis. This is the most common small vessel vasculitis. In children it can occur as a reaction to a drug or infection, particularly group A β-haemolytic streptococcal infection, but in some cases there is no identifiable trigger. It is, however, more common in adults than children. It typically presents as palpable purpura, with or without a maculopapular rash. The lesions themselves may be more common in areas of trauma, dependency or tight clothing, and are most often seen on the legs.1 The rash itself tends not to be highly symptomatic and, although the associated arthralgia is uncomfortable, patients are usually not systemically unwell. There is a characteristic appearance on skin biopsy, with inflammation of the vessel wall and a neutrophilic infiltrate.
- Henoch–Schönlein purpura. This is a relatively common small vessel vasculitis, and it is more common in children than adults. The condition presents with characteristic palpable and erythematous purpura, and typically affects the buttocks and lower limbs. The rash is often accompanied by arthralgia and abdominal pain but other features may be present, such as urticaria, vesicles and even skin ulceration. Orchitis may occur in boys. Associated renal involvement is common.2 On skin biopsy, IgA immune complex deposition is observed in the vessel wall. This is characteristic, and sets Henoch–Schönlein purpura apart from other vasculitides.
- Viral exanthem. Viral illnesses can cause a purpuric skin eruption associated with systemic symptoms, such as fever, arthralgias and malaise. The viruses most commonly implicated are cytomegalovirus, hepatitis B and C viruses, Epstein–Barr virus and parvovirus B19.
- Meningococcal septicaemia with meningitis. This is the most important condition to be considered in this clinical scenario, and it was the correct diagnosis for the patient described above. There should be a high level of concern for meningococcal septicaemia in a patient who is unwell and presents with a purpuric rash and headache. Vomiting and diarrhoea may also occur. Early on, the lesions may look more like macules or papules, but as they progress and haemorrhage the typical petechial or purpuric eruption appears.3 The characteristic appearance of the purpura can be due to thrombocytopenia or localised or disseminated intravascular coagulation, or to direct vascular damage from the meningococcal organism or from immune complex deposition.4 The appearance of the typical purpuric rash is a sign of advancement of the disease and is associated with higher morbidity.
Investigations
A diagnosis of meningococcal septicaemia is confirmed through culture of Neisseria meningitidis from blood and/or cerebrospinal fluid. If antibiotic therapy has already been commenced, PCR testing can be performed. A full septic work-up is required to determine the extent of any multisystem organ dysfunction, particularly hepatic and renal impairment. However, in the acute setting it may not be appropriate to conduct a lumbar puncture, and one of the contraindications in this case would be the possibility of a coagulopathy. Any investigations should not delay commencement of antibiotic therapy.
Treatment
Immediate treatment is required for all suspected cases of meningococcal disease. Empirical antibiotic therapy with cefotaxime, ceftriaxone or benzylpenicillin should be administered as soon as possible, along with dexamethasone, which reduces the risk of secondary sequelae from meningitis. Close contacts should be given appropriate chemoprophylaxis.
References
1. Fiorentino DF. Cutaneous vasculitis. J Am Acad Dermatol 2003; 48: 311-340.
2. Jennette JC, Falk RJ, Andrassy K, et al. Nomenclature of systemic vasculitides. Proposal of an international consensus conference. Arthritis Rheum 1994; 37: 187-192.
3. Toews WH, Bass JW. Skin manifestations of meningococcal infection; an immediate indicator of prognosis. Am J Dis Child 1974; 127: 173-176.
4. Kingston ME, Mackey D. Skin clues in the diagnosis of life-threatening infections. Rev Infect Dis 1986; 8: 1-11.

