What’s the diagnosis?
A severe blistering eruption in an elderly patient
Case presentation
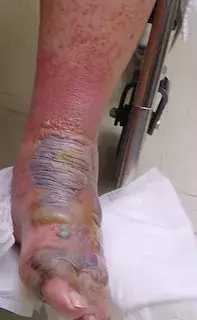
A 75-year-old man presents with a severe blistering eruption on his ankle and foot (Figure 1). He recently suffered a small cut on the ankle and began to self-treat it with a herbal cream containing rhus extract. Four days later the eruption developed. It is intensely itchy and is starting to appear on other parts of his body, including the skin on his face and penis.
Differential diagnosis
Conditions to include in the differential diagnosis include the following.
- Bullous impetigo. This skin infection, caused by Staphylococcus aureus, is usually of sudden onset and is characterised by superficial bullae that range in size. As the infection progresses the bullae rupture, leaving erosions with yellow-brown crusting. It is sore and can spread rapidly to involve other areas of skin. Bullous impetigo is itchy, but not usually intensely so.
- Bullous pemphigoid. This autoimmune blistering skin disease almost always occurs in elderly patients. For the patient described above, features that are suspicious for bullous pemphigoid include his age, the presence of large, tense bullae and the associated pruritis. However, when blistering occurs it is typically on a base of normal skin (rather than inflamed skin), which did not occur in this case. Many patients with bullous pemphigoid report a prodrome of itching and eczematous erythematous lesions prior to the development of blisters. Diagnosis is made by lesional and perilesional skin biopsy with immunofluorescence – this will show a subepidermal blister, usually with an eosinophilic infiltrate with IgG and C3 deposits at the dermoepidermal junction.
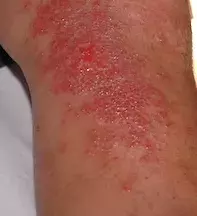
- Allergic contact dermatitis. This is the correct diagnosis. The lesions of allergic contact dermatitis are highly variable in appearance but are usually erythematous and oedematous (Figure 2). Blistering is common and sometimes dramatic with bullae formation, as occurred in this case. The lesions are characterised by intense pruritis and can be painful when the blisters rupture. The most common primary sites involved are the hands, feet, eyelids and lips, which commonly come into contact with allergens.
Causes
Allergic contact dermatitis is caused by a wide range of substances. Allergens can be found in plants and in almost any type of commercial preparations, such as personal care products, topical medications, household cleaning agents and chemicals in the workplace. Some of the most common allergens in applied substances include neomycin, balsam of peru, perfumed products and thimerosal. Plants and plant products are often implicated, particularly the rhus tree (Toxicodendron succedaneum) and plants from the Grevillea genus. Nickel sulfate is a common cause of allergic contact dermatitis, which manifests as persistent itchy rashes on skin that is in contact with jewellery, metal studs, watchbands and earrings.
Aetiology
Allergic contact dermatitis results from a delayed type IV hypersensitivity reaction. The period between initial exposure to a substance and the appearance of a skin reaction is typically a number of days. Once a patient has been sensitised to an allergen, subsequent reactions may occur much more quickly upon re-exposure. Upon repeated exposure to allergens, a sensitised individual can develop chronic skin disease – this is usually marked by lichenified, confluent, erythematous plaques with variable hyperkeratosis, crusting scale and fissuring. The eruption is initially limited to the areas exposed to the substance and may spread to surrounding skin, particularly if the area is occluded or sweaty. In this patient’s case, the allergen was easily spread to other parts of the body by the hand that had been applying the rhus extract, and this caused the rash to develop on distal sites such as the face and penis.
Investigations
A diagnosis of allergic contact dermatitis is usually made on the basis of a detailed history of exposure and clinical examination. Nonetheless, it would be appropriate to take a culture of any scale or exudate from the surface of the lesion to exclude a fungal or bacterial infection. If there is suspicion of another condition, such as bullous pemphigoid, then a skin biopsy would be helpful. Patch testing will confirm a diagnosis of allergic contact dermatitis and, if required, should be performed at least two weeks after ceasing any corticosteroids (these drugs may produce false negative results). However, for the patient described in this case, the allergen was clearly identified and could easily be avoided, so skin biopsy and patch testing were not necessary.
Management
Treatment of an acute, localised eruption caused by allergic contact dermatitis requires potent topical corticosteroids with wet dressings and regular emollients. An oral antihistamine is also useful to reduce itch. If the eruption is severe and widespread, a short course of an oral corticosteroid may be required and is rapidly effective, provided that the patient has no contraindications to these medications.
In the long term, management requires avoidance of the allergen, which in this case involved avoidance of the rhus tree itself and any products containing rhus extract. The rhus tree is a known cause of allergic contact dermatitis and has been declared a noxious weed in Australia for this reason, but rhus extract can still be found in some herbal preparations.
Further reading
NSW Department of Primary Industries. NSW Weedwise. Rhus tree (Toxicodendron succedaneum). Available at: www.dpi.nsw.gov.au/agriculture/pests-weeds/weeds/profiles/rhus (accessed September 2015).
Australasian Society of Clinical Immunology and Allergy. Contact dermatitis (ASCIA education resources (AER) patient information. Available at: http://www.allergy.org.au/patients/skin-allergy/contact-dermatitis (accessed September 2015).
Allergy

