What’s the diagnosis?
Bullae in an older man after a fall
Case presentation
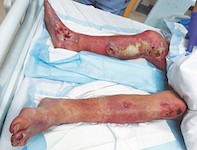
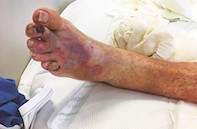
A 68-year-old man is referred to the hospital emergency department by his primary care physician with worsening bullae on both legs (Figures 1a and b). He had a fall one week earlier in his backyard and is unsure how long he was immobilised. He does not recall any injuries after this event, but that evening he noticed a blister on the instep of his right foot. He was initially treated with cephalexin, but over the next few days he developed further bullae across both legs, which easily burst. These bullae are not associated with significant pain or pruritus and he has not used any other new medications. He has a medical history of atrial flutter and type 2 diabetes which is treated with insulin. His social circumstances are poor.
On examination, a bilateral polymorphic bullous eruption is observed. There is geometrical figurate erythema around the right medial knee bullae. On lower limb neurological examination, his sensation is intact to touch, heat, cold and vibration and he has normal propioception. He has no diabetic foot ulcers. He is tachycardic, with a heart rate of 128 beats per minute, but otherwise stable and afebrile.
Investigations reveal raised inflammatory markers, with a C-reactive protein level of 176 mg/mL and a white cell count of 12.2 x109/L. He is in a significant hyperosmolar hyperglycaemic state with a blood glucose level of 26 mmol/L and serum osmolarity of 339 mmol/L. Long-term control of his diabetes has been very poor, as evidenced by a HbA1c of 9.9%.
Treatment is initiated with empirical intravenous antibiotics, fluid resuscitation and an insulin infusion.
Differential diagnoses
Conditions to consider for a patient with bullous disease of the lower limb include the following.
- Bullous pemphigoid (BP). This autoimmune chronic blistering disease usually occurs in older patients. Potential causes include infections and drugs such as dipeptidyl peptidase-4 inhibitors.1 The pathophysiology involves antibodies towards structural components of the hemidesmosomes that maintain the structural integrity of the skin.2 It typically begins with eczematous lesions that are pruritic and develop into tense bullae that are distributed widely, including on the trunk, extremities, axillae and groin. BP is diagnosed with skin biopsy, which typically shows eosinophilic spongiosis, subepidermal blistering and superficial inflammatory cell infiltrates; immunofluorescence on the biopsy shows linear antibody deposition along the basement membrane.3 Blood tests for antibodies to the specific hemidesmosomal proteins BP180 and BP230 are also used in the diagnosis.
- Burn injuries. These injuries have various causes, including heat, chemicals, friction and electricity, and were considered in this case because of the erythema surrounding the ulcers and their geometrical nature. Body surface area affected in a patient with a burn injury can be calculated using the rule of nines, excluding areas affected superficially (epidermal involvement only).4 If over 10% of the total body surface area is involved, a burn is considered a systemic injury and an inflammatory response can cause significant fluid loss and hypovolaemic shock – fluid resuscitation must be commenced as soon as possible with reference to the Parkland formula.4
- Bullous diabeticorum. This rare cutaneous complication of diabetes is difficult to definitively exclude – it has no specific diagnostic test and is often underdiagnosed.5 It presents without a clear precipitant and involves tense subepidermal bullae in a diabetic patient with noninflamed skin. The bullae are often large and nontender, and occur over acral areas on the lower limbs.6 The histopathological features are nonspecific and include intraepidermal or subepidermal blisters, spongiosis and nonspecific inflammation.
- Coma blisters. This is the correct diagnosis. Coma blisters are subepidermal bullae that occur on sites of pressure secondary to immobilisation. The pathophysiology is poorly understood, but it is presumed that focal pressure secondary to immobilisation in combination with toxic effects of drugs can cause rapid local hypoxia and necrosis.7 Risk factors include causes of prolonged immobilisation: drug overdose (classically with barbiturates),8 hypoglycaemia, head trauma, diabetic ketoacidosis and neurological diseases (e.g. stroke and peripheral nerve diseases).9 Clinically, the condition begins with plaques and bullae that develop rapidly on sites of pressure 48 to 72 hours after immobilisation and are usually self-limiting, improving within one to two weeks after mobilisation resumes.10,11
Investigations
For a patient with suspected coma blisters, biopsy is important to rule out other potential causes like BP. Histopathological examination for coma blisters typically contains evidence of intraepidermal blisters, eccrine sweat gland necrosis and thrombosis of vessels in the upper dermis. Inflammatory infiltrate can be mild to moderate and neutrophils are sparsely found in the dermis.12
Management
As coma blisters are self-limiting in nature, management is focused on the underlying risk factors and causes. In addition, frequent wound care and dressing changes are vital to prevent secondary wound issues. If the wounds become complicated by infection, it is important to involve a multidisciplinary team with infectious diseases specialists for appropriate antibiotics, surgeons for potential debridement and specialist nursing staff for optimal wound care and dressings.
Outcome
For this patient, a punch biopsy showed nonspecific findings, including patchy spongiosis of the epidermis, isolated necrotic keratinocytes with no confluent epidermal necrosis and focal intracorneal clefting at the edge of the biopsy. The overall morphology, temporal association with immobilisation, rapid evolution and distribution of the bullae is consistent with a diagnosis of coma blisters. Wound swabs grew Staphylococcus argenteus, and the patient was treated with ongoing intravenous antibiotics. Wound care measures were implemented by nursing staff in the hospital. Unfortunately, the patient’s wounds were complicated and he required an extended hospital admission and wound debridement by plastic surgeons.
In this case, aggressive management of the patient’s hyperosmolar hyperglycaemic diabetes was important to prevent dehydration and electrolyte issues, as well as to optimise the wound healing environment. Ongoing investigations include blood glucose monitoring and assessment of osmolarity to ensure biochemical improvement.
References
1. García-Díez I, Ivars-Lleó M, López-Aventín D, et al. Bullous pemphigoid induced by dipeptidyl peptidase-4 inhibitors. Eight cases with clinical and immunological characterization. Int J Dermatol 2018; 57: 810-816.
2. Kasperkiewicz M, Zillikens D, Schmidt E. Pemphigoid diseases: pathogenesis, diagnosis, and treatment. Autoimmunity 2012; 45: 55-70.
3. Schmidt E, della Torre R, Borradori L. Clinical features and practical diagnosis of bullous pemphigoid. Dermatol Clin 2011; 29: 427-438, viii-ix.
4. Moore RA, Waheed A, Burns B. Rule of nines. In: StatPearls [internet]. Treasure Island FL: StatPearls Publishing; 2020-. PMID: 30020659.
5. Chatterjee D, Radotra A, Radotra BD, Handa S. Bullous diabeticorum: a rare blistering manifestation of diabetes. Indian Dermatol Online J 2017; 8: 274-275.
6. Ghosh SK, Bandyopadhyay D, Chatterjee G. Bullosis diabeticorum: a distinctive blistering eruption in diabetes mellitus. Int J Diabetes Dev Ctries 2009; 29: 41-42.
7. Dinis-Oliveira RJ. Drug overdose-induced coma blisters: pathophysiology and clinical and forensic diagnosis. Curr Drug Res Rev 2019; 11: 21-25.
8. Spillane JD. Bullous lesions in acute barbiturate intoxication. BMJ 1965; 1: 1308.
9. Sami N, Yeh SW, Ahmed AR. Blistering diseases in the elderly: diagnosis and treatment. Dermatol Clin 2004; 22: 73-86.
10. Rocha J, Pereira T, Ventura F, Pardal F, Brito C. Coma blisters. Case Rep Dermatol 2009; 1: 66-70.
11. Chacon AH, Farooq U, Choudhary S, et al. Coma blisters in two postoperative patients. Am J Dermatopathol 2013; 35: 381-384.
12. Sánchez Yus E, Requena L, Simón P. Histopathology of cutaneous changes in drug-induced coma. Am J Dermatopathol 1993; 15: 208-216.
Skin conditions
Diabetes complications

