What’s the diagnosis?
A toddler with recurrent itchy nodules on the legs
Case presentation
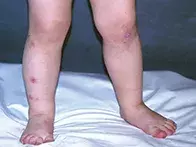
A 15-month-old boy presents with recurrent itchy lesions on his legs (Figure). He scratches them and they rapidly become excoriated and infected. It is summer time, and his mother says he has been bitten by mosquitoes on several occasions. She has noticed that these mosquito bites often develop a large wheal that takes several days to resolve.
Conditions to include in the differential diagnosis for a child of this age include the following.
- Recurrent impetigo. This superficial infection of the epidermis is caused by Staphylococcus aureus or Streptococcus pyogenes. Impetigo is common in children secondary to minor skin trauma, especially when there is impaired barrier function such as in a patient with atopic dermatitis. It usually begins as small erythematous lesions, which develop a serous and purulent discharge and then typical golden or brown crusting. In most cases, the lesions are localised, but they may spread rapidly and can be itchy or painful. For the child described above who has a history of insect bites, impetigo is a diagnosis to consider, but it is not likely because it does not typically develop a wheal. Localised impetigo can be self-limiting, but it resolves promptly with oral or topical antibiotics. However, when a carrier state is established (as often occurs in children who have recurrent lesions) it recurs quickly after antibiotic treatment is ceased.
- Atopic dermatitis. This condition is very common in young children and is characterised by erythematous, scaly and pruritic lesions on the cheeks and the extensor surfaces of the arms and legs. The skin involvement tends to be widespread. Children tend to have lesions that are not well defined and are surrounded by dry skin. Bacterial infection is common secondary to scratching. For the child described above, who has a small number of lesions on the legs with normal surrounding skin, it is not the most likely diagnosis.
- Prurigo. This chronic skin condition is characterised by multiple, extremely itchy hyperkeratotic papules and nodules. The initial lesion can be caused by an insect bite or another form of irritation and inflammation. In the early stages the lesion is flat and erythematous, but with chronic excoriation and rubbing it becomes nodular, up to 3 cm in diameter and usually irregular in shape. Secondary infection can occur. The most commonly affected body sites are the legs, face, trunk and arms, which can easily be rubbed and scratched. Some children who suffer from chronic itchy skin diseases, including eczema and psoriasis, can develop prurigo secondary to scratching. Prurigo is not seasonal and it is characterised by persistent lesions.
- Dermatitis artefacta. The lesions of dermatitis artefacta are secondary to a deliberate action that inflicts physical trauma to the skin. The lesions are asymptomatic and may appear well demarcated and bizarre in shape, and they are almost always located in areas that are easily reached, such as the hands, face, arms and legs. They tend to heal quickly. The history of how the lesions occurred and progressed is often vague or difficult to believe. Dermatitis artefacta may indicate an underlying psychological illness or distress; it may also be a consequence of attention-seeking behaviour or of a child being unable to express himself or herself verbally. Self-inflicted skin disease is very unlikely in small children, but dermatitis artefacta can be a sign of child abuse.
- Papular urticaria. This is the correct diagnosis. Papular urticaria occurs predominately in young children after exposure to a foreign protein in an insect bite, usually from a mosquito or flea.1,2 On initial exposure there may not be a reaction but the patient develops immune sensitisation to the foreign protein. On the next exposure, there is a delayed type IV hypersensitivity reaction that leads to itchy papules or nodules. Each time the patient is bitten by the insect subsequently, all previous lesions are reactivated. This may occur hours to days after the bite, and eventually a patient may have ongoing lesions at all times. It can be very confusing for the parents.
Presentations
True urticaria is, by definition, an evanescent process. The term ‘papular urticaria’ is a misnomer, as the reaction can last days to weeks. It may be possible initially to see a punctum mark within the wheal that marks the area of trauma, but because the lesions are intensely itchy they rapidly become excoriated and secondarily infected with bacteria. Severe lesions can have blisters or even be ulcerated.
Lesions caused by a flying insect will often be limited to exposed skin, such as the legs and arms, whereas lesions caused by insects that can crawl under clothing (e.g. fleas, ticks, mites) can occur anywhere on the body. Papular urticaria caused by mosquitoes is characteristically seasonal.
There can also be an immediate type I reaction to the insect bite prior to the onset of the subsequent type IV reaction. This explains the wheal that this patient’s mother described. It can present quite a confusing clinical picture.
Management
Most cases of papular urticaria are mild. The condition tends to be self-limiting because children usually become desensitised to the foreign protein after one to two years. For patients who have persistent itchy, superinfected lesions, however, it is important to break the itch and scratch cycle. Potent topical corticosteroids, such as betamethasone dipropionate 0.05%, are most effective. A nonsedating antihistamine can be helpful to reduce the initial wheal and histamine-mediated flare response. Bacterial superinfection should be treated with antibiotics. Swabs from skin lesions frequently return Staphylococcus aureus; however, treating this organism alone is ineffective because it is not the primary cause of the problem.
It is important to determine the causative organism and to protect the child from insect bites where possible. Suitable strategies may include the use of personal insect repellent and protective clothing (particularly when outside in the evening when mosquitoes are problematic) and insect-proof bed netting. Parents may be concerned that insect repellents are harmful to their child’s skin, but they can usually be persuaded to apply it to clothes and hair. Pest control agents may be needed in the house. If there are pets in the home that may be carrying fleas then it may be necessary to seek veterinary advice regarding treatment with a systemic agent.
It is important to reassure parents that papular urticaria is a benign and self-limiting process. Many parents describe the origin of different types of children’s rashes as ‘bites’. In the case of papular urticaria, they are correct.
References
1. Millikan LE. Papular urticaria. Semin Dermatol 1993; 12: 53-56.
2. Howard R, Frieden IJ. Papular urticaria in children. Pediatr Dermatol 1996; 13: 246-249.
Skin lesions

