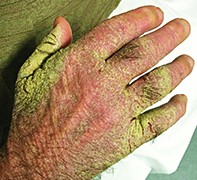
Thick warty crusts on the hands
Test your diagnostic skills in our regular dermatology quiz. What is the cause and appropriate management of the thick warty crusts on this man’s hands?
Case presentation
A 45-year-old man presents with thick warty crusts on the dorsal and palmar surfaces of both hands (Figures 1a and b). The eruption has been present for three months and is slightly itchy. There is also a brown discolouration of his fingernails.
The rash has been treated with topical corticosteroids but the patient believes these have made the rash worse. Blood tests have been performed and show blood eosinophilia.
Differential diagnoses
Conditions to consider among the differential diagnoses include the following.
- Psoriasis. Psoriasis may be limited to the hands. It presents with erythema, lichenification, scale and often nail dystrophy. Pustules and fissures may be present; itch is variable. However, the case patient described above has reported that his symptoms worsened when treated with topical corticosteroids, which is not typical of psoriasis. It is uncommon for psoriasis to be limited to the palms, and brown nail discolouration is not typical.
- Tinea of the hands. Tinea involving the hands may present with scale, erythema and lichenification. If a nail dystrophy is present then there is commonly subungual debris and destruction of the nail plate. The infection is usually caused by the dermatophyte Trichophyton rubrum; most patients have a pre-existing foot infection with or without toenail involvement. Poor peripheral circulation and palmar keratoderma are predisposing factors. It is characteristic for tinea to be asymmetrical in distribution, and it is unilateral in about half of cases. Fungal culture of skin scrapings and nail clippings will confirm the diagnosis.
- Chronic hand dermatitis. This typically occurs in atopic people who are exposed to occupational irritants, such as hairdressers, carpenters and cleaners. It presents as a chronic, pruritic eczema that is hyperkeratotic and papulovesicular. The nails may be mildly ridged but not severely dystrophic. It is unlikely to be the diagnosis for the patient described above, who is not chronically exposed to irritants and whose rash is of only three months’ duration. In addition, his nail discolouration is not consistent with a diagnosis of chronic hand dermatitis.
- Genetically-determined palmoplantar keratoderma. There are many genodermatoses that can result in unusual hyperkeratosis of the hands (and usually also the feet). These include Darier’s disease, hidrotic ectodermal dysplasia, pachyonychia congenita and Greither palmoplantar keratoderma. It would be unlikely for any of these genetic conditions to present for the first time in the fifth decade of life. Most patients have other cutaneous features, as well as involvement of the feet.
- Crusted scabies. This is the correct diagnosis. Crusted scabies (previously known as Norwegian scabies) is a type of scabies in which very large numbers of Sarcoptes scabiei mites are present. Patients with ordinary scabies have only a few mites, probably because their burrows are destroyed when the skin is scratched. Crusted scabies occurs in people with an inadequate immune response to the mite, which allows the parasite to multiply. There is variation in individual susceptibility, and not all patients are immunosuppressed. It is a severe disease that has a significantly higher morbidity than ordinary scabies.
Investigations
A diagnosis of crusted scabies is readily confirmed by examination of skin scrapings, which will be teeming with mites and eggs. Dermoscopy may also reveal the mite at the end of a burrow.
Management
Crusted scabies is more resistant to treatment than ordinary scabies. Treatment with topical permethrin cream alone requires repeated applications and the failure rate is significant.
The treatment of choice for crusted scabies is oral ivermectin (200 µg/kg), which is highly effective and should be given weekly. A keratolytic agent, 6% salicylic acid in an emollient base, should be applied nightly under damp cotton gloves to reduce hyperkeratosis. Hands are washed in the morning and the crusts debrided using a nail brush to remove scale. A topical scabicidal agent, 5% permethrin cream, is applied to the hands daily, and reapplied each time the hands are washed. Once a week, the scabicidal agent should also be applied to the entire skin (i.e. the whole body) and left on for 24 hours; nails should be cut short and brushed with the same agent and then the nail brush washed thoroughly in hot water. Oral and topical treatments are used for three to four weeks until clinical resolution occurs and, ideally, a repeat scraping from the hands is negative.1
In addition to treating the infestation, it is important to control the associated itch, which often persists after treatment is completed due to a hypersensitivity reaction to the scabies mites and their faeces and eggs.2 Paradoxically, itch in crusted scabies is often milder than in ordinary scabies. Topical corticosteroids are useful in treating itch, but a short course of oral prednisone may be used after the infestation has been cleared to treat itch that is severe and persistent.
Contact tracing is mandatory for all patients with scabies. The risk of disease transmission to other people by physical contact is high, especially for crusted scabies. If possible, individuals who have been in contact with the patient should be treated, including household contacts. The case patient described above lives in a remote Aboriginal community, where he works as a nurse, and it is likely that he has acquired the parasite at work. Scabies is endemic in Aboriginal communities in the Northern Territory and is a difficult problem, with health workers being at risk of contracting the infestation. Useful information is provided in guidelines developed by the Department of Health, Northern Territory for the Healthy Skin Program, a resource that is available online (see www.health.nt.gov.au/library/scripts/objectifyMedia.aspx?file=pdf/10/83.pdf).3 MT
References
- Chouela EN, Abeldaño AM, Pellerano G, et al. Equivalent therapeutic efficacy and safety of ivermectin and lindane in the treatment of human scabies. Arch Dermatol 1999; 135: 651-655.
- Currie BJ, McCarthy JS. Permethrin and ivermectin for scabies. N Engl J Med 2010; 362: 717-725.
- Healthy skin program. Guidelines for the community control of scabies, skin sores, tinea and crusted scabies in the Northern Territory. Darwin: Centre for Disease Control, Department of Health, Northern Territory; 2015. Available online at: http://hdl.handle.net/10137/698 (accessed May 2017).
COMPETING INTERESTS: None.