What’s the diagnosis?
An area of cutaneous atrophy on the abdomen

Case presentation
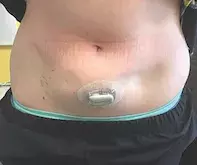
A 14-year-old girl presents with an area of marked cutaneous atrophy on her left lower abdomen that has developed over the last three months (Figure 1). Before this the skin was normal, with no preceding rash or oedema. She has been otherwise well and denies any trauma to the affected area.
The patient was diagnosed with type 1 diabetes mellitus at age 13 years, for which she is treated with insulin glargine and insulin aspart via a subcutaneous insulin pump. She recalls the area of atrophy as a site where her insulin pump was previously situated.
There is no family history of venous thromboembolism or of autoimmune disease.
Differential diagnoses
The lipodystrophies are a heterogeneous group of diseases characterised by an abnormal change in adipose tissue, which may be either an increase (lipohypertrophy) or decrease (lipoatrophy). This patient’s age and the morphology of the lipoatrophy and lack of visible changes to adipose tissue bulk in other areas are consistent with an acquired localised lipoatrophy. Causes to consider among the differential diagnoses include the following.
- Trauma. Chronic pressure and trauma can result in pressure-induced localised lipoatrophy caused by decreased adipose tissue perfusion.1 Lipoatrophy semicircularis is a rare form of acquired localised lipoatrophy in which individuals develop bilateral, circumferential band-like depressions on the anterolateral thighs; its cause is unknown but repeated microtrauma due to occupational exposures has been purported to play a contributing role.2
- Panniculitis. Lipoatrophy may be a remnant of previous panniculitis, as well as the primary feature in lipoatrophic panniculitis and dermatomyositis-induced panniculitis.3,4 Lipoatrophic panniculitis presents with tender erythematous plaques and nodules that develop into circumferential bands of lipoatrophy that, unlike in this case, are symmetrical and preferentially involve the distal extremities.3 Lipoatrophic lesions in the context of dermatomyositis tend to be multifocal and develop without any antecedent inflammatory skin changes but may still be accompanied by a symmetrical proximal myopathy; biopsy specimens of these areas demonstrate a lobular panniculitis with an overlying histiocytic dermal and perivascular infiltrate.5 Lupus erythematosus panniculitis (LEP) initially presents with groups of tender subcutaneous plaques and nodules that preferentially involve the proximal extremities, trunk, face and scalp.4 In the acute phase of LEP, the skin surface of these nodules may exhibit erythema, dyspigmentation or ulceration; these nodules resolve over time, resulting in localised lipoatrophy with scarring.4 Biopsy of an acute LEP lesion would demonstrate a predominantly lobular panniculitis with fat necrosis, calcification, dermal mucin and immunoglobulin G/complement C3 deposition along the dermoepidermal junction.4
- Morphoea. Also known as localised scleroderma, morphoea is a rare idiopathic disease of the skin and subcutaneous tissue characterised by progressive fibrosis due to abnormal collagen deposition (Figure 2).6 Morphoea is distinguished from the more sinister diagnosis of systemic sclerosis by being a localised disease of the skin with the absence of accompanying telangiectasia, Raynaud’s phenomenon, nailfold capillary abnormalities and visceral involvement. Morphoea has a female predominance and affects children and adults equally. Morphoea may occur as patches or as linear lesions, with the linear form being the more common variant in children.6 Lesions can be solitary or multiple and appear initially as inflammatory plaques and patches with overlying erythema involving the trunk and extremities that over time become hyperpigmented. These lesions eventually settle into white areas with a characteristic surrounding violaceous edge that may appear atrophic. Biopsy features are dependent on the stage of the lesion being sampled – early lesions demonstrate perivascular lymphocytes, plasma cells and eosinophils in the reticular dermis with accompanying collagen thickening and endothelial cell swelling, whereas late lesions show a paucity of inflammatory cells, atrophic eccrine glands and thickened, crowded collagen bundles.6
- Iatrogenic lipoatrophy. Subcutaneous injection of medications can induce localised lipoatrophy. In a case series of 16 patients with idiopathic localised lipoatrophy, 10 patients had a history of subcutaneous medication injection at the site of lipoatrophy before its onset.7 The medications injected included (in order of frequency): corticosteroids, antibiotics and methotrexate.7 The biopsy features from this case series identified small adipose lobules with a reduced number and size of adipocytes, with accompanying prominent vessels and a paucity of inflammatory infiltrate.7
- Insulin lipoatrophy. This is the correct diagnosis. Subcutaneously injected insulin results in lipodystrophy in 0.1 to 3% of diabetic individuals, with lipohypertrophy being the most common type.8 The exact mechanism underlying insulin-induced lipoatrophy is unknown, but a role for TNF-alpha induced release of lysosomal enzymes has been proposed.8 In addition, high titres of anti-insulin antibodies and increased deposition of immunoglobulin M, complement C3 and fibrinogen at the periphery of lipoatrophic lesions points to an underlying hypersensitivity reaction to insulin.8,9 Since the use of purified human insulins has become more widespread, the prevalence of lipoatrophy has reduced to less than 10% among diabetic patients who develop a lipodystrophy.9 Lipoatrophy usually develops at sites of regular injection after six months of treatment and, once developed, rarely resolves spontaneously.9 Biopsy shows lobules of hypoplastic adipocytes, lymphocytic infiltrate and hyperplastic capillaries.8
Diagnosis and management
For this patient, the history of insulin injection at the site and absence of trauma and other subcutaneous injections or systemic features concerning for autoimmune or connective tissue disease made insulin-induced lipoatrophy the likely diagnosis. Biopsy was not offered.
The chance of spontaneous resolution of the atrophic area is rare and treatment options directed toward increasing adipose tissue bulk include injection of purified human insulin to the edge of the atrophic area, as well as a combination of subcutaneously injected dexamethasone (4 mcg per unit of insulin) and insulin.9 A small case series has demonstrated the efficacy of subcutaneous cromolyn injections, a mast-cell stabilising agent, in reversing early insulin-induced lipoatrophic skin lesions, implicating a pathogenic role of mast cells in the development of these lipoatrophic changes.10 Diabetic patients with lipoatrophy have also experienced resolution of atrophic lesions following commencement of continuous subcutaneous insulin infusion with human purified insulins.8
Outcome
The girl and her parents were advised that she should avoid further subcutaneous insulin injection to the affected site and to change the site of the insulin pump daily. In liaison with paediatric endocrinologists, her insulin was changed to insulin lispro, a human insulin analogue. The atrophic area to the left abdomen improved, with subsequent resolution over the following 12 months.
References
1. Hussain I, Garg A. Lipodystrophy syndromes. Endocrinol Metab Clin North Am 2016; 45: 783-797.
2. Gómez-Espejo C, Pérez-Bernal A, Camacho-Martínez F. A new case of semicircular lipoatrophy associated with repeated external microtraumas and review of the literature. J Eur Acad Dermatol Venereol 2005; 19: 459-461.
3. Shen LY, Edmonson MB, Williams GP, Gottam CC, Hinshaw MA, Teng JM. Lipoatrophic panniculitis: case report and review of the literature. Arch Dermatol 2010; 146: 877-881.
4. Fraga J, García-Díez A. Lupus erythematosus panniculitis. Dermatol Clin 2008; 26: 453-463, vi.
5. Commens C, O’Neill P, Walker G. Dermatomyositis associated with multifocal lipoatrophy. J Am Acad Dermatol 1990; 22(5 Pt 2): 966-969.
6. Fett N, Werth VP. Update on morphea: part I. Epidemiology, clinical presentation, and pathogenesis. J Am Acad Dermatol 2011; 64: 217-228.
7. Dahl PR, Zalla MJ, Winkelmann RK. Localized involutional lipoatrophy: a clinicopathologic study of 16 patients. J Am Acad Dermatol 1996; 35: 523-528.
8. Radermecker RP, Piérard GE, Scheen AJ. Lipodystrophy reactions to insulin: effects of continuous insulin infusion and new insulin analogs. Am J Clin Dermatol 2007; 8: 21-28.
9. Richardson T, Kerr D. Skin-related complications of insulin therapy: epidemiology and emerging management strategies. Am J Clin Dermatol 2003; 4: 661-667.
10. Lopez X, Castells M, Ricker A, Velazquez EF, Mun E, Goldfine AB. Human insulin analog-induced lipoatrophy. Diabetes Care 2008; 31: 442-444.
Diabetes type 1

