What’s the diagnosis?
Asymptomatic facial rash in a boy
Case history
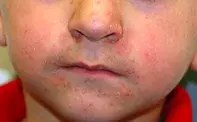
An 8-year-old boy presents with an asymptomatic but unsightly facial rash that has been present for nine months (Figure 1). It is confined to the skin around his mouth, on the sides of his nose and below his eyes (where there are a few papules).
When the rash first appeared, the patient was treated with 1% hydrocortisone cream. This suppressed the rash initially, but when treatment was ceased the rash recurred and subsequently became resistant to the cream. Topical miconazole was ineffective. Topical mometasone furoate 0.1% cream was initiated. Again there was a good initial response, but this was lost with ongoing treatment and attempts to cease the treatment resulted in increasingly severe flares of the rash.
Diagnosis
The correct diagnosis in this case is periorificial dermatitis (POD), a common condition also known as perioral dermatitis. It is harmless and asymptomatic but unsightly. In adults it is quite common, usually the result of applying potent corticosteroids to the facial skin, but in children it often starts as an idiopathic condition that is then worsened by topical corticosteroid use.
The hallmark of POD is the distribution around the mouth, sides of the nose and under the eyes. A close look at the morphology of the rash reveals it to be micropapular, erythematous, scaly and pustular. Swabs from the pustules do not yield pathogens.
Cause
The cause of POD is essentially unknown. However, some authors have suggested that it may represent a form of childhood rosacea.1,2
Differential diagnosis
Conditions that should be considered in the differential diagnosis include the following.
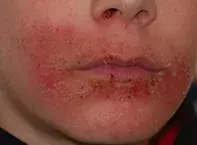
- Irritant and allergic contact dermatitis is the condition that is most commonly confused with POD. However, the rash is confluent, itchy and scaly (Figure 2), without the papules and pustules that are characteristic of POD. There is frequently a history of a contact irritant such as a dummy, comforter, musical instrument or another object held to the mouth. Food intolerance may sometimes cause this clinical picture.
- Folliculitis may cause diagnostic confusion because of the presence of pustules. The majority of cases are caused by Staphylococcus aureus; a bacterial swab will rule this out.
- Tinea may be both scaly and pustular. However, a distribution around the mouth resembling that of POD would be very unusual. A skin scraping for fungal microscopy and culture will exclude this diagnosis.
Treatment
Although it is not an infection, POD responds to oral antibiotics from the tetracycline and macrolide groups. However, treatment needs to be prolonged and usually requires a minimum of six weeks of continuous treatment. The most commonly used antibiotic in children is erythromycin; tetracyclines may be used in children over 8 years of age. The antibiotic is prescribed at half the dosage used to treat bacterial infections.
Topical antibiotics are sometimes effective but treatment must also be prolonged. Those most commonly used are erythromycin and clindamycin. Both are available as acne medications.
It is essential to cease topical corticosteroid treatment. This usually results in an initial flare that can be severe and last up to two weeks. Patients must be warned that this is likely because it can be quite alarming.
Prognosis
It is not uncommon for POD to recur. If this happens, it is important to remember not to restart topical corticosteroids and to instead treat the rash with antibiotics. Indeed, patients who are prone to POD should avoid using topical corticosteroids on the face at all. However, the prognosis is good.
Keypoint
In children, POD is often missed as a diagnosis and it is not uncommon for the condition to persist for many months. Careful attention to the distribution and morphology of the rash will enable GPs to make the right diagnosis at the first presentation.

