What’s the diagnosis?
Painful nodules and plaques on the lower legs
Case presentation
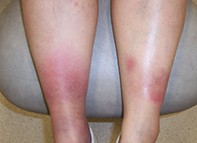
An 18-year-old woman presents with painful nodules and plaques on her lower legs (Figure). She also complains of arthralgia involving her ankles.
The patient is afebrile and otherwise well. She has recently commenced the oral contraceptive pill but she takes no other medications.
Diagnosis
The correct diagnosis in this case is erythema nodosum, which is the most common type of panniculitis. It is characterised by bilateral painful and erythematous nodules or plaques of sudden onset, which tend to affect the anterior legs, particularly the shins, knees and ankles. Ulceration is rare, but as the lesions evolve they become more bruise-like in appearance. Accompanying arthralgia, malaise and fever are common. Erythema nodosum most commonly affects women under the age of 40 years.1
Discussion
Panniculitis is a general term for an uncommon array of disorders that primarily involve inflammation of the subcutaneous fat and result in deep inflammatory nodules and plaques. Some types of panniculitis are characterised by ulceration, atrophy or sclerosus, and the skin often feels firm and indurated. There is also discolouration of overlying skin, which can vary from a redness to brown. The lesions are sometimes tender. As they heal, there may be residual scarring and atrophy due to lipodystrophy. Differentiating the many types of panniculitis involves a tissue biopsy to a depth of adipose tissue, as well as tissue culture.
Erythema nodosum has a specific histopathology: septal panniculitis without vasculitis (inflammation of the fibrous septae between fat lobules). It occurs as a result of a hypersensitivity reaction to a specific antigen or in association with other medical conditions, such as inflammatory bowel disease and sarcoidosis. The most common identifiable antigenic stimulus is group A streptococcal pharyngitis, but tuberculosis and Yersinia infections are also implicated. Drugs may trigger erythema nodosum – for the patient described above, the precipitant was almost certainly the commencement of the oral contraceptive pill, which is one of the best described causes of this reaction pattern. Other precipitants include pregnancy, autoimmune disorders and malignancies. In about one-third of patients no cause is found.
For the patient described above, cellulitis should be included in the differential diagnosis. This infection of the lower dermis and subcutaneous fat is usually caused by group A streptococcus or Staphylococcus aureus. The lesions of cellulitis are more likely to be asymmetrical and less well demarcated than the lesions visible for this patient, and cellulitis is more likely to be unilateral than bilateral. Cellulitis is characteristically tender and erythematous, as in this case, but patients often feel unwell and are febrile with evidence of lymphadenopathy. Patients with lower leg cellulitis often have a portal of entry of infection, which is commonly tinea pedis.
Investigations
Often, the typical acute onset of lesions, which evolve from an initial red to bruised appearance, is sufficiently characteristic for a clinical diagnosis of erythema nodosum to be made. However, it is important to investigate potential causes, especially if the patient is showing systemic signs of illness. Basic inflammatory markers should be evaluated, with a full blood count and C-reactive protein measurement in addition to a liver function test. If there is suspicion of a streptococcal pharyngitis, a throat swab and antistreptolysin-O titre (ASOT) would be appropriate. A chest x-ray should be arranged if there is any reason to suspect the association with tuberculosis and sarcoidosis, and patients should be examined for other signs that could indicate such systemic diseases.
The duration of erythema nodosum is typically three to six weeks. For patients with lesions that continue to erupt for longer periods (chronic erythema nodosum), other causes of panniculitis need to be considered. In this setting, a biopsy is indicated, using a deep elliptical incision technique to sample subcutaneous fat. Such biopsy sites on the lower legs should be sutured to ensure adequate healing.
Management
The lesions of erythema nodosum are generally self-limiting and resolve over three to six weeks without any residual scarring or atrophy. However, any clearly identifiable cause, such as a medication, should be addressed (for this patient, it was stopping the oral contraceptive pill). The treatment of any underlying illness is important but does not necessarily correlate with improvement of erythema nodosum, and the lesions are likely to improve regardless.
Simple NSAIDs are appropriate for symptomatic relief. If patients are incapacitated by joint pain or are very unwell, a short course of prednisone is rapidly effective. Other medications, such as dapsone, potassium iodide and colchicine (off-label uses), have been used to treat erythema nodosum, particularly if the condition is chronic. In the situation where erythema nodosum is not self-limiting, referral to a dermatologist is recommended.
Reference
1. Cribier B, Caille A, Heid E, Grosshans E. Erythema nodosum and associated diseases. A study of 129 cases. Int J Dermatol 1998; 37: 667-672.
Skin lesions

