What’s the diagnosis?
Purpura after physical activity

Case presentation
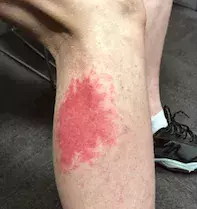
A 61-year-old man presents with a new, asymptomatic cutaneous eruption involving his right calf (Figure 1a). He is systemically well, without fever, arthralgia or abdominal pain, and he denies any obvious triggers, such as infectious symptoms, new medications or trauma.
The erythematous patch with petechiae occurred one day after the patient visited the Sydney Royal Easter Show, where he spent the majority of the day walking during warm weather. He has a sedentary lifestyle and comments that the amount of walking and time spent on his feet was ‘out of the norm’ for him. His background medical history is remarkable for Crohn’s disease, for which he was treated with ustekinumab for two years.
On examination, the patient is afebrile and normotensive. Cutaneous review reveals three distinct erythematous, non-blanching foci of his right calf, admixed with subtle petechial change.
Investigations are arranged, and normal results are returned for full blood count; urea, electrolytes and creatinine levels; liver function tests; C-reactive protein level and erythrocyte sedimentation rate. Further test results are unremarkable for antinuclear antibody and antineutrophil cytoplasmic antibody level, complement levels (C3 and C4) and coagulation studies. Urinalysis does not reveal any microscopic haematuria; in addition, urine microscopy, culture and sensitivity, and an analysis for red cells, casts and dysmorphic cells are negative.
A punch biopsy from the involved skin is performed, and histological examination reveals red blood cell extravasation, endothelial cell swelling and a perivascular neutrophilic infiltrate consistent with leukocytoclastic vasculitis (LCV) – see Figure 1b.
Differential diagnoses
Cutaneous vasculitis can present in a subtle nondistinct fashion in its early phase before progressing to frank purpura. The following conditions should be considered among the differential diagnoses for a patient presenting with a purpuric lesion of the lower limb.
- Cutaneous small-vessel vasculitis. Small vessel vasculitis can present with isolated involvement of the skin; it can also present with manifestations of systemic vasculitis such as fever, weight loss, myalgia and renal involvement. Identified causes include infections (15 to 20% of patients), autoimmune diseases (15 to 20%), hypersensitivity drug reactions (10 to 15%) and paraneoplastic disorders (5% or less); however, about 50% of cases are idiopathic.1 Infectious associations include hepatitis B, hepatitis C, group A streptococcus infection and chronic bacteraemias (e.g. infective endocarditis).2 Implicated drugs include beta lactams, cephalosporins, sulphonamides and ustekinumab. Associated autoimmune conditions include systemic lupus erythematosus, rheumatoid arthritis and inflammatory bowel disease. The pathophysiology involves immune complex deposition in small vessel walls and activation of inflammatory pathways.3 Clinical features include palpable nonblanching purpura/petechiae on the skin. Systemic vasculitides that should be excluded include polyarteritis nodosa, granulomatosis with polyangiitis, microscopic polyangiitis and eosinophilic granulomatosis with polyangiitis. Once systemic involvement has been excluded, the aim of management is symptomatic relief. Histological examination of cutaneous small-vessel vasculitis reveals LCV.
- Senile purpura. Also known as actinic purpura, this is a benign recurrent cause of ecchymosis and purpura on the extensor surfaces after minor trauma. Risk factors include increasing age, sun exposure and the use of corticosteroids and anticoagulants. Management focuses on preventive measures such as sun protection.4
- IgA vasculitis. Previously known as Henoch-Schönlein purpura, this condition typically affects younger patients but it can occur at any age. It presents as an acute small-vessel vasculitis with palpable purpura, occasionally with systemic involvement of the gastrointestinal tract (abdominal pain) and joints (arthralgia). The aetiology is poorly understood and may correlate with infectious triggers such as Streptococcus pyogenes.5 IgA vasculitis is typically self-limiting when only the skin is involved. Skin biopsy reveals LCV and direct immunofluorescence of perilesional skin shows the presence IgA antibodies, confirming the diagnosis.6 Supportive treatment with topical corticosteroids for the skin is usually sufficient; however, systemic involvement often warrants systemic corticosteroid therapy and occasionally steroid-sparing agents, pending progress and the clinical course. Renal involvement can occur and requires monitoring even after the cutaneous involvement has resolved.6
- Urticarial vasculitis. This form of vasculitis initially presents with urticarial skin lesions that typically last more than 24 hours (in contrast to standard urticaria) and are followed by a purpuric stain. It is typically associated with connective tissue diseases like systemic lupus erythematosus. There are normo- and hypocomplementaemic subtypes, with the latter typically associated with systemic involvement.7 Histopathology demonstrates LCV. Patients with systemic symptoms and extensive cutaneous involvement can be treated with corticosteroids, colchicine (off-label), NSAIDs or hydroxychloroquine (off-label).
- Capillaritis. This condition is sometimes known as pigmented purpuric dermatitis and as Golfer’s capillaritis. Capillaritis presents with a pigmented purpuric eruption of the lower limbs, but on biopsy there is usually no true vasculitis. It can develop after exercise, as a reaction to medications or as a result of an infection.8
- Exercise-induced vasculitis (EIV). This is the correct diagnosis. Exercise can cause a benign small-vessel vasculitis that presents with purpuric lesions on the lower limbs. EIV typically presents with a polymorphous eruption of macular, urticarial or purpuric lesions.9 The lesions may be asymptomatic or associated with itch, pain or a burning sensation. It typically occurs in older patients after prolonged exercise or standing on warmer days (which promotes vasodilation). Increasing age, heat and prolonged exercise are likely aetiological factors and the pathophysiology may be related to venous stasis and subsequent vascular inflammation.8,9 Histopathology demonstrates LCV with red blood cell extravasation, endothelial cell swelling and perivascular neutrophilic infiltrate.10 EIV is also known as golfer’s vasculitis: in one study, 15 of 17 patients with the condition (88%) developed it in association with playing golf.11 It was more likely to occur in older patients (mean age, 53 years) when the whole 18 rounds of golf were played (more than three hours of physical activity) and generally only during summer months.9,11
Management
EIV typically resolves spontaneously. General recommendations for management include temporarily reducing physical activity, elevating affected limbs and using compression socks or stockings.10 However, in some cases compression can exacerbate the eruption by increasing heat and caution should be exercised in patients with peripheral vascular disease.9 Symptomatic relief can be achieved with potent topical corticosteroids.12
EIV frequently recurs, especially after similar provoking circumstances of prolonged exercise during warm weather.9 Evidence for prevention is limited and strategies are based on the hypothesised aetiological factors. These include wearing lighter clothing to prevent overheating, using compression stockings to reduce venous stasis and avoiding prolonged exercise during hot weather.9,12
Outcome
For this patient, supportive care was initiated with topical corticosteroids and emollient. He was advised to rest and to elevate the leg when possible. On follow-up review one week later, the cutaneous lesions had completely resolved and he remained systemically well.
The patient’s history of prolonged physical activity in warm conditions prior to presentation, the morphology of the eruption, rapid and spontaneous resolution, biopsy findings and negative blood and systemic screen support the diagnosis of EIV. It is important to consider other vasculitides when evaluating patients with purpuric eruptions of the lower limbs and to rule out any serious causes with appropriate investigations.
References
1. Goeser MR, Laniosz V, Wetter DA. A practical approach to the diagnosis, evaluation, and management of cutaneous small-vessel vasculitis. Am J Clin Dermatol 2014; 15: 299-306.
2. Marzano AV, Vezzoli P, Berti E. Skin involvement in cutaneous and systemic vasculitis. Autoimmun Rev 2013; 12: 467-476.
3. Shavit E, Alavi A, Sibbald RG. Vasculitis – what do we have to know? A review of literature. Int J Lower Extrem Wounds 2018; 17: 218-226.
4. Ceilley RI. Treatment of actinic purpura. J Clin Aesthet Dermatol 2017; 10: 44-50.
5. Weiss PF, Klink AJ, Luan X, Feudtner C. Temporal association of Streptococcus, Staphylococcus, and parainfluenza pediatric hospitalizations and hospitalized cases of Henoch-Schönlein purpura. J Rheumatol 2010; 37: 2587-2594.
6. Hetland LE, Susrud KS, Lindahl KH, Bygum A. Henoch-Schönlein purpura: a literature review. Acta Derm Venereol 2017; 97: 1160-1166.
7. Hamad A, Jithpratuck W, Krishnaswamy G. Urticarial vasculitis and associated disorders. Ann Allergy Asthma Immunol 2017; 118: 394-398.
8. Oakley A. Capillaritis. DermNet NZ; Oakley A (ed.); 2016. Available online at: https://dermnetnz.org/topics/capillaritis (accessed September 2021).
9. Espitia O, Dréno B, Cassagnau E, et al. Exercise-induced vasculitis: a review with illustrated cases. Am J Clin Dermatol 2016; 17: 635-642.
10. Wu B. Exercise-induced vasculitis. In: DermNet NZ; Oakley A (ed); 2015. Available online at: https://dermnetnz.org/topics/exercise-induced-vasculitis (accessed September 2021).
11. Prins M, Veraart JC, Vermeulen AH, Hulsmans RF, Neumann HA. Leucocytoclastic vasculitis induced by prolonged exercise. Br J Dermatol 1996; 134: 915-918.
12. Kelly RI, Opie J, Nixon R. Golfer’s vasculitis. Australas J Dermatol 2005; 46: 11-14.

