What’s the diagnosis?
Sudden onset of blistering lesions in a young boy

Case history
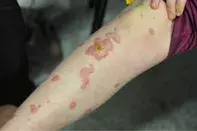
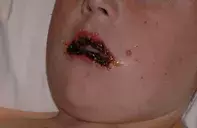
A 12-year-old boy presents with sudden onset of blistering lesions on his arms and legs (Figures 1a and b), occurring a few days after he developed a typical cold sore on his upper lip. What is the most likely diagnosis?
Diagnosis and differential diagnosis
The diagnosis in this case is erythema multiforme. Careful observation of these blisters show that they have the morphology of ‘target lesions’. Although not every lesion demonstrates this, most have a red areola, then an area of grey with a red centre. True target lesions are highly characteristic of erythema multiforme.
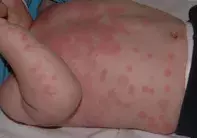
The most common condition confused with erythema multiforme is urticaria, which may be ‘targetoid’, as shown in Figure 2, but careful observation reveals that these lesions are in fact simply annular. Differentiating erythema multiforme from urticaria is straightforward. The lesions in urticaria never blister and always migrate if observed over several hours. Erythema multiforme lesions are fixed and last up to two weeks. However, both conditions are often acute in onset.
Other causes of blistering rashes include bullous impetigo, other viral exanthemata and tinea.
Clinical spectrum and causes
Erythema multiforme has a wide clinical spectrum ranging from a benign blistering rash involving only the arms and legs to a widespread life-threatening eruption causing severe erosions of all mucosal surfaces, including the conjunctivae.
Many cases of erythema multiforme are the result of a recent herpes simplex infection such as a cold sore; however, infections with Mycoplasma pneumoniae may also result in severe erythema multiforme. Less often, drug eruptions may result in the same type of rash.
When caused by herpes simplex infection, erythema multiforme often recurs with each attack. This can be highly disruptive as the rash lasts for about two weeks.
Confirming the diagnosis
Erythema multiforme has a very characteristic skin biopsy appearance. Histology will also rule out other causes of blistering eruptions. Blistering lesions should be swabbed for bacterial culture. Once the diagnosis is established all new medications should be stopped and antibody titres for mycoplasma requested.
It is often difficult to prove a recent herpes simplex infection as these can be subclinical, serology can be unreliable and there may be no obvious lesion from which to take a sample for viral culture. However, because herpes simplex is such a common cause it is not unreasonable to assume such infection is responsible until proven otherwise.
Management
In mild cases, particularly when there has been a clear history of a recent herpes simplex infection, patients should be given oral antiviral medication and, to mitigate the severity of the attack, oral prednisone.
If the patient is unwell and has severe mucosal involvement, he or she should be admitted to hospital and commenced on intravenous aciclovir and a macrolide antibiotic to cover the possibility of mycoplasma infection until titres are available. In these severe cases, the literature suggests that prednisone is unhelpful; however, supportive care of the patient needs to be maximal and multidisciplinary, often necessitating admission to a high dependency or intensive care unit.
Prognosis
With good care patients have an excellent prognosis but in those with recurrent disease due to herpes simplex virus infection, oral long-term antiviral prophylaxis is required.

