What’s the diagnosis?
An erythematous pustular rash on the torso and limbs

Case presentation
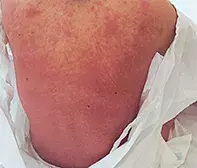
A 29-year-old woman presents to the emergency department after a pre-syncopal episode that occurred while she was showering. She has been unwell for approximately two weeks with a flu-like illness that has progressed to a cough. She developed a rash approximately one week before her presentation. The rash has become erythematous and confluent across her torso and limbs (Figure 1a). The erythema is studded with small pustules.
The patient is febrile and unwell but has a normal level of consciousness. She is noted to have a markedly raised neutrophil count of 18.0x109 cells/L (normal range, 2.0x109 to 7.0x109 cells/L). Other blood parameters are normal.
The woman had a thyroidectomy for thyroid cancer two weeks previously and is recovering well. Her regular medications are thyroxine and calcium supplements. While she was unwell with the flu-like illness, she says she had taken one course of antibiotics and she had started a cough syrup for her productive cough in the last week.
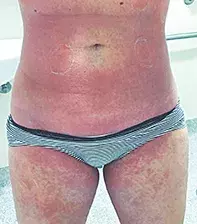
She is admitted to hospital for investigation and treatment. The rash starts to desquamate during her admission (Figure 1b).
Differential diagnoses
Conditions to consider among the differential diagnoses include the following.
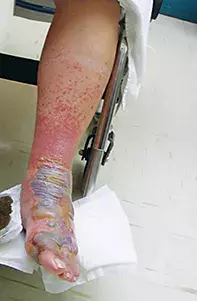
- Allergic contact dermatitis. Allergic contact dermatitis is typically characterised by well demarcated, erythematous eruptions that are intensely pruritic. The reaction can be patchy or diffuse for allergens that are applied to a large area. Vesicles and blisters frequently occur in contact dermatitis (Figure 2), but pustules are not typically a feature. Patients are itchy but not unwell and there is no change in blood count. It is not likely to be the diagnosis for the case patient, who had no history of contact with a new topical agent.
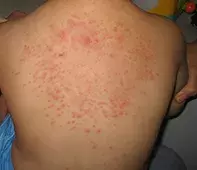
- Folliculitis. This is the classic eruption that causes widespread pustules (Figure 3). Folliculitis is most often a Staphylococcus aureus infection. It may be caused by other agents, including Pityrosporum and Pseudomonas organisms, but not usually as an acute event. The pustules are usually individual lesions, not occurring on a wide background of erythema, and the patient is well, afebrile and does not have neutrophilia. Swabs typically return Staphylococcus aureus. A sterile folliculitis characterised by eosinophils can also occur in patients with HIV disease.
- Drug reaction with eosinophilia and systemic symptoms (DRESS). Also known as drug hypersensitivity syndrome, this is a rare and severe reaction to a drug. As opposed to other drug reactions, DRESS develops two to eight weeks after the commencement of the causative medication. The most commonly associated drugs are antiepileptics, allopurinol, olanzapine and sulfonamides. Patients who have DRESS present with a fever, morbilliform rash, lymphadenopathy and inflammation of one or more major organs. Additionally, haematological abnormalities are often present; these include eosinophilia, atypical lymphocytes, thrombocytopenia and anaemia. The rash in patients with DRESS has varying morphology and may include target lesions and pustules. For the case patient, this diagnosis was not likely because her eosinophils were not deranged, there was no evidence of major organ involvement, and she developed the rash less than one week after starting antibiotics and cough syrup.
- Stevens–Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN). SJS and TEN are dermatological emergencies. Both commence with fever and an acute erythematous eruption that progresses to blistering. In patients with TEN there is also sheeting off of large areas of skin. SJS is most commonly triggered by herpes simplex and Mycoplasma pneumoniae. TEN is most commonly secondary to drugs, with the most common causes being antiepileptics, sulfonamides, allopurinol and NSAIDs. The rash is characterised by mucous membrane involvement of the mouth, vagina, rectum and eyes. The skin is acutely erythematous and painful.
- Pustular psoriasis. This is a rare acute exanthematic form of psoriasis characterised by an erythematous eruption studded with sterile pustules (Figures 4a and b). The skin is moderately painful. Patients are not acutely unwell but may have a fever and rigors due to loss of temperature control. A moderate neutrophilia may be present. Approximately 10% of patients who develop pustular psoriasis have a background of chronic psoriasis. Pustular psoriasis is triggered by the sudden tapering of corticosteroids, drugs (lithium, aspirin, indomethacin) or infection.
- Acute generalised erythematous pustulosis (AGEP). This is the correct diagnosis. AGEP is an uncommon skin eruption characterised by the rapid development of an erythematous rash with superficial sterile pustules. The rash typically starts around the face but becomes widespread, and it is worse in the skin folds. AGEP is secondary to drugs in 90% of cases, with the most common causes being beta-lactams, tetracyclines, sulfonamides and antifungal agents. However, pholcodine, which is found in some cough syrups, has been implicated.1,2 This was the responsible agent in this case. Viral infections are implicated in children. The rash typically starts two to four days after exposure to the causative agent. Patients are typically quite unwell and febrile with a very high white cell count, which is higher than would be expected from a bacterial infection.
Investigations
AGEP is diagnosed on the basis on the history, characteristics of the rash, increased neutrophil count and skin biopsy. A biopsy specimen consistent with AGEP demonstrates sterile pustules filled with neutrophils, which was the case in this patient. It is also important to identify the causative medication or virus. Patch testing may be performed to identify the drug responsible, but it can usually be inferred due to the short time between exposure and the development of the rash.
Pustular psoriasis can be very difficult to differentiate from AGEP because the clinical and biopsy characteristics are similar, as occurred in this patient. Differentiation lay in the preceding history of medications and illness.
Management
The first and most important step of management in AGEP is to stop the medication responsible. As AGEP can be precipitated by over-the-counter medications, it is important to ask about these specifically. Prednisone may be commenced to speed resolution, but the rash will resolve spontaneously once the offending drug is ceased, in approximately 10 days. Supportive management is indicated to relieve symptoms, and is accomplished through use of emulsifying ointment, topical corticosteroid ointments, wet wraps and oral antihistamines.
Outcome
The patient’s condition improved with prednisone 0.5 mg/kg/day, topical betamethasone dipropionate ointment and emulsifying ointment plus oral antihistamines. She was discharged home well after five days.
References
1. Kline A, Fischer G. Acute generalised exanthematous pustulosis and other severe drug eruptions from over the counter medications: a case report and review of the literature. Australas J Dermatol 2016; 57: 92-96.
2. Lee S, Artemi P, Holt D. Acute generalized exanthematous pustulosis. Australas J Dermatol 1995; 36: 25-27.

