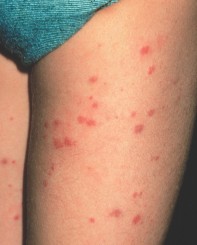
Purpuric rash: is it meningococcal disease?
A young boy who was under observation for suspected early appendicitis one day ago has developed a purpuric rash on his buttocks and thighs. How do you assess his condition and decide on appropriate management?
Case scenario
Ahmed is a 6-year-old boy, in good health, of normal height and weight who has been developing normally. On Friday, he developed abdominal pain. Early appendicitis was considered and he was sent to the local emergency department for review and observation.
After eight hours there was no shift in the location of the pain and Ahmed did not have a fever. He was sent home with paracetamol for pain relief to be reviewed by his GP. On Saturday evening, his parents noticed a purpuric, nonblanching rash over his buttocks that extended down the back of his legs. He passed a very dark stool. As the on-call doctor for your practice, you are asked to see him.
- What is the likely diagnosis?
- How should you treat Ahmed?
- What is the prognosis?
Commentary
Ahmed has a fairly typical presentation of Henoch-Schönlein purpura (HSP), the most common childhood vasculitis. Although HSP is mainly a condition of young school-age children it can also occur in infants, adolescents or adults, with a worse prognosis.1 HSP is caused by immune-complex deposition in the skin. Other common names for HSP include IgA vasculitis, anaphylactoid purpura and purpura rheumatica.
Features of Henoch-Schönlein purpura
Three key features differentiate HSP from other similar conditions. These are the rash type and distribution, arthritis and abdominal pain.
Characteristics of the rash are:
- gravity or pressure-dependent distribution on the buttocks and lower limbs
- palpable purpura as distinct from viral exanthems such as measles, which are flat
- nonblanching.
Meningococcal bacteraemia also presents this way, but the child would be extremely unwell if they had an HSP distribution of meningococcal rash; they would almost certainly be febrile, and they would hopefully already be in an ICU. Children with HSP are relatively well apart from the abdominal pain and are almost always afebrile. If a diagnosis of HSP is being considered in a febrile child, a second opinion should be sought, cultures taken and empiric antibiotic therapy started first. Children with meningococcal disease can be reasonably well in the very early stages but their condition can deteriorate quickly. Management of a reasonably well afebrile child with typical HSP features does not require cultures and antibiotic therapy.
One of the most common features of HSP is arthritis. Again, this usually involves the lower limbs (ankles and knees), but the elbows can also be affected.
The abdominal pain associated with HSP is often colicky in nature and can be quite severe. The major condition to exclude is intussusception. Intussusception can be caused by any condition where there is inflammation of the gastrointestinal tract but is particularly common in HSP. The palpable purpura seen in the skin is also evident in the lining of the gut, predisposing it to become a lead point for intussusception. Ahmed has blood in the stool, but no other features of intussusception were noted. An abdominal ultrasound would be useful to exclude intussusception if there was any doubt.
Other classic features of HSP may be noted but are not required for the diagnosis. These include the presence of blood (occasionally macroscopic) or protein on urinalysis and hypertension, which is usually mild.
There may be a history of a preceding illness, but this is of no particular use as most children have such a history. However, it is worthwhile to exclude any recent medication use.
Diagnostic tests
HSP is one of the few paediatric conditions where no investigations are warranted other than urinalysis.2 A full blood count would exclude idiopathic thrombocytopenic purpura, but so would a history and examination (no other signs of HSP, and petechiae on the upper body and/or oral mucosa). Leukaemia is exceedingly unlikely unless there are other features (e.g. prolonged illness with weight loss, organomegaly or lymphadenopathy). A biopsy will confirm the presence of IgA and C3 complement deposits in the skin (or kidney), although the main thing it will confirm is that the clinician was uncertain about the diagnosis. There are only very few conditions for which a C-reactive protein test or erythrocyte sedimentation rate are indicated, despite the number that are ordered in tertiary teaching hospitals, but HSP is not one of those conditions.
Very few cases of HSP can be linked to a definitive cause, although perhaps ‘trigger’ is a preferable term as the exact aetiology of this condition is unknown. If any other organ such as the brain or lung is affected (e.g. haemoptysis, dyspnoea, neurological findings or severe headache), urgent referral to a paediatric specialist and further investigations are mandatory.
Treatment
Symptomatic treatment is the mainstay of this condition but NSAID use should be avoided if the patient has gastrointestinal bleeding. The use of corticosteroids is controversial. A 2015 Cochrane review of interventions for preventing and treating kidney disease in patients with Henoch-Schönlein purpura found that in 13 trials including 1403 patients there was no benefit of two to four weeks of prednisone to prevent kidney disease.3 In my view the risks of a few weeks of corticosteroids (usually 1 mg/kg daily, maximum 60 mg) outweigh the benefits, but many paediatricians use a brief course followed by a weaning plan because the child will feel better when taking prednisone. Heparin appeared to be effective in reducing the risk of persistent kidney disease in one trial, but the side effects of heparin are concerning and its use is not supported given the low risk of renal complications. Cyclophosphamide was ineffective in preventing progressive kidney injury.
Prognosis
The outcome is almost always very good in children, but it can be a difficult few weeks or months until the condition resolves. Although the major concern is renal impairment, if present, it is usually transient. However, it is important to advise parents that one-third of children will have at least one relapse, usually in the first two months. Renal impairment is almost always evident within two months, so the guidelines recommend regular urinalyses for three months (weekly if results are abnormal and fortnightly if results are normal), then at six and 12 months.2 Blood pressure monitoring at each review is also recommended. Paediatric specialist review is required if there are atypical features, lung or brain involvement (e.g. haemoptysis, dyspnoea, neurological findings or severe headache), proteinuria, macroscopic haematuria or hypertension, or any abnormalities on blood tests (if these were done for some reason).
Conclusion
Most cases of Henoch-Schönlein purpura are self-limiting and require only symptomatic management such as paracetamol or NSAIDs if they are not contraindicated due to gastrointestinal bleeding. Renal involvement can be asymptomatic, and close follow up is crucial for identifying significant renal involvement requiring intervention. MT