What’s the diagnosis?
Multiple crusted lesions on the scalp
Case presentation
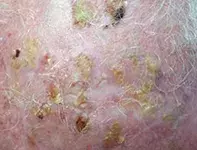
A 78-year-old man presents with multiple crusted irritable lesions on his scalp that he says have been slowly worsening over the past year (Figure). The lesions are irritable, causing him to pick and scratch. He has generalised sun damage and has had a history of actinic keratoses, basal cell carcinoma (BCC) and squamous cell carcinoma (SCC).
Differential diagnosis
Conditions to consider in the differential diagnosis include the following.
- Erosive pustular dermatosis of the scalp. This chronic condition is characterised by sterile pustules that become progressively eroded, crusted and irritable. There may be associated alopecia in affected areas. It can be difficult to distinguish from an area affected by skin cancers and is differentiated from an overlying infection by the absence of infective features (such as oedema and warmth), negative bacterial swabs and lack of improvement with antibiotic therapy. Biopsy shows epidermal erosion, infiltration of inflammatory cells in the dermis and destruction of hair follicles. Although the cause is unknown, local trauma and sun damage are thought to predispose patients to the condition. It responds to potent topical corticosteroids and sun protection.
- Cicatricial pemphigoid. This blistering skin condition is a rare variant of bullous pemphigoid. It commonly affects the mucosal membranes of the genitals, oral cavity and conjunctiva, but it can occur on any part of the skin, especially the scalp, face and upper trunk. Cicatricial pemphigoid occurs predominantly in the elderly population and is more common in women. Biopsy shows evidence of blistering in the dermal–epidermal junction and linear deposition of various autoantibodies such as IgG, IgA, C3 and C4 at the basement membrane zone. It is treated with oral or topical corticosteroids and immunosuppressive medications.
- Actinic damage with hyperkeratotic actinic keratoses and infection. This is the correct diagnosis, and it is much more common than either of the conditions discussed above. The lesions begin as erythematous macules or papules and develop a rough, dry and scaly surface. Although commonly asymptomatic, they can become painful and increasingly irritable as they increase in size – this can lead patients to pick at the lesions and cause them to ulcerate and become superinfected and pustular. Histologically, an actinic keratosis is a hyperkeratotic cutaneous lesion consisting of atypical keratinocytes and is a potential precursor for invasive SCC. It most commonly occurs on areas of the skin that are chronically exposed to UV radiation, such as a bald scalp and the face and hands; there are often multiple lesions in an affected region.
Management
For a patient presenting with a suspected bacterial superinfection of an actinic keratosis, a bacterial swab should be taken in the first instance and any infection (which is usually caused by Staphylococcus aureus) should be treated with antibiotics. A biopsy should be performed to rule out erosive pustular dermatosis. In addition, any suspicious hyperkeratotic lesion with an indurated base should be biopsied to rule out SCC.
There are many management options for actinic keratosis and the optimal approach will depend on the extent, location, number of lesions and the general health and wishes of the patient. Localised lesions are managed with liquid nitrogen cryotherapy, curettage and cautery or photodynamic therapy. Dispersed lesions that cover a large area are often managed with 5-fluorouracil cream, which is a topical chemotherapeutic agent, or with topical imiquimod, which initiates an inflammatory cascade that specifically targets and causes apoptosis of dysplastic keratinocytes while sparing normal skin. Both of these ‘field therapies’ usually cause quite severe local irritation at the time of application but can be very effective – they also have the advantage of self-application, noting that it is important to assess an elderly patient’s home support before prescribing them. Other topical therapies include salicylic acid and diclofenac.
Patients who have a large number of actinic keratoses are at significantly increased lifelong risk of melanoma and nonmelanoma skin cancer and should therefore have a regular full skin examination. In general, this examination should be performed every six to 12 months, although for patients with severe actinic damage it may need to be more frequent. They should also be educated about the importance of sun protection measures. In a patient such as the elderly man described above, daily use of a sunscreen that is easy to apply, such as an aerosol spray formulation, coupled with wearing a hat when outdoors, would be the best advice.
Outcome
For this patient, the skin infection was first treated with oral antibiotics and the crusts were debrided with the aid of salicylic acid cream. This was followed by treatment with topical 5-fluorouracil for three weeks. Individual hyperkeratotic lesions were treated with a combination of cryotherapy and curettage. One lesion proved to be a SCC and was excised. When treatment had been completed and his scalp was normal, the patient was advised to apply sunscreen every day and to wear a hat when outdoors, and because of the severity of his scalp lesions and past history of nonmelanoma skin cancer, to present for a medical examination every three months.
Skin cancer
Sun exposure

