What’s the diagnosis?
A teenager with a blistering skin eruption
Case presentation
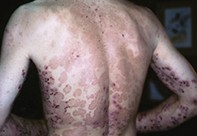
An 18-year-old man presents with a three-month history of a severe itchy, blistering eruption involving his trunk, upper limbs and oral mucosa (Figure). He had been previously well. At first presentation, skin swabs had been taken and demonstrated Staphylococcus aureus. The patient had been treated with two courses of oral flucloxacillin, but the eruption has not improved. What is the most likely diagnosis?
Differential diagnosis
Conditions that should be considered in the differential diagnosis include the following:
- Bullous impetigo. This skin infection is caused by release of exfoliative toxin A from certain strains of S. aureus. It is characterised by superficial blisters that rupture and crust, leaving erythematous circular patches. A skin swab confirms the diagnosis, and it responds to appropriate antibiotic therapy.
- Bullous pemphigoid. This autoimmune blistering disease is characterised by pruritis, erythematous lesions and large tense blisters. It typically occurs in people over the age of 60 years and is extremely rare in children and adolescents. Bullous pemphigoid is usually associated with IgG antibodies directed against the epidermal basement membrane.
- Dermatitis herpetiformis. This IgA-mediated autoimmune blistering disease, which may occur in adolescence, is characterised by long-term blistering and pruritis. It is associated with gluten-sensitive enteropathy, which may not be suspected at the time when a patient presents with the blistering skin eruption. Dermatitis herpetiformis tends not to present with such widespread blistering as shown in the case described above. The eruption is often most obvious on the elbows, knees and buttocks.
- Linear IgA disease. This is the correct diagnosis in the patient described above. A rare autoimmune blistering disorder, linear IgA disease occurs most commonly in children (also termed chronic bullous disease of childhood) and young adults, but it can occur in people of any age. There is a bimodal peak of presentation in post-pubertal adolescence and age over 60 years.1,2 IgA autoantibodies act against basement membrane antigens, but linear IgA disease is not associated with gluten-sensitive enteropathy. The blistering may be widespread and may involve mucosal surfaces, including the conjunctivae. The condition is usually idiopathic but has been associated with infection, local skin trauma, antibiotics (particularly penicillins and vancomycin) and some other drugs.3,4
Diagnosis
Diagnosis of linear IgA disease (and indeed all immunobullous diseases) is by skin biopsy with direct immunofluorescence. Demonstration of the characteristic IgA deposition in a linear fashion at the basement membrane will differentiate linear IgA disease from other blistering conditions.3
Taking a skin swab is a very reasonable first step in a patient presenting with a bullous disease because immunobullous disorders are all much rarer than bullous impetigo. However, a lack of response to flucloxacillin will alert the doctor to the fact that the finding of S. aureus was a secondary phenomenon. The finding of a positive swab for S. aureus is common in longstanding skin diseases where the epidermis has been disrupted.
Treatment
Linear IgA disease is characteristically difficult to treat. First line treatment is dapsone;2 sulfasalazine can be added if there is a limited response to dapsone alone. Some patients may also require low-dose oral prednisone. Referral to a dermatologist is recommended for a patient who presents with a persistent blistering skin disease.
References
1. Wojnarowska F, Marsden RA, Bhogal B, Black MM. Chronic bullous disease of childhood, childhood cicatricial pemphigoid, and linear IgA disease of adults. A comparative study demonstrating clinical and immunopathologic overlap. J Am Acad Dermatol 1988; 19(5 Pt 1): 792-805.
2. Fortuna G, Marinkovich MP. Linear immunoglobulin A bullous dermatosis. Clin Dermatol 2012; 30: 38-50.
3. Guide SV, Marinkovich MP. Linear IgA bullous dermatosis. Clin Dermatol 2001; 19: 719-727.
4. Whitworth JM, Thomas I, Peltz SA, Sullivan BC, Wolf AH, Cytryn AS. Vancomycin-induced linear IgA bullous dermatosis (LABD). J Am Acad Dermatol 1996; 34(5 Pt 2): 890-891.
Skin lesions
Skin conditions

