Multiple inflammatory nodules on the hands
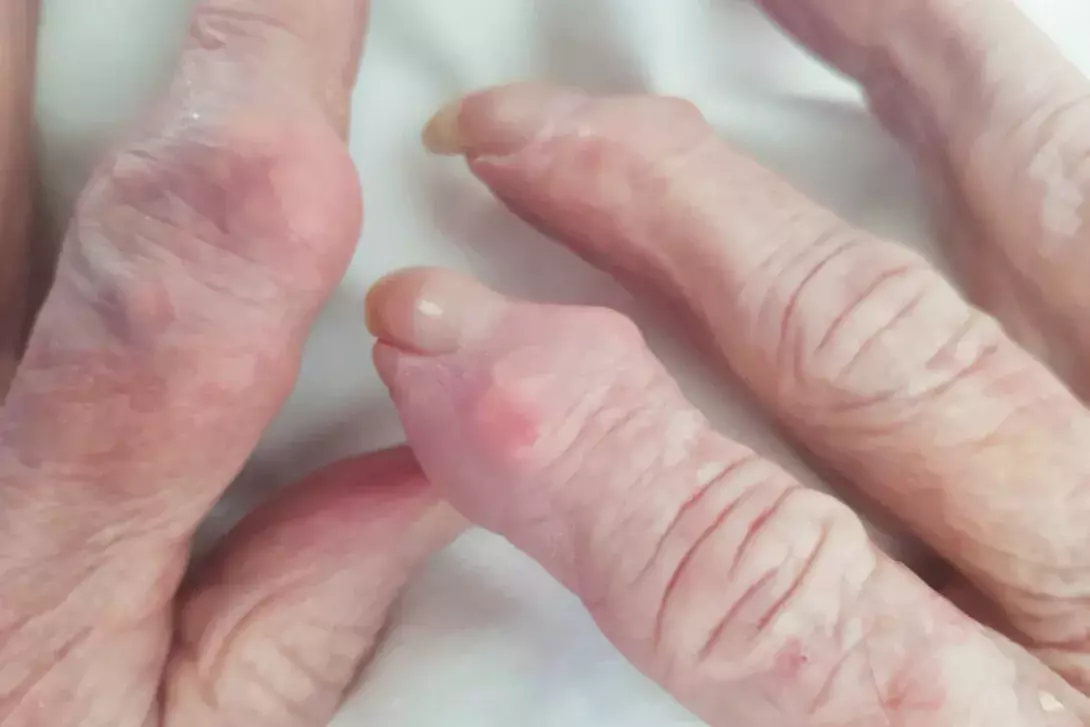
Test your diagnostic skills in our regular dermatology quiz. What is the cause of these nodules, which are located on the extensor surface of the interphalangeal joints of a woman’s fingers?
Case presentation
A 75-year-old woman presents for a full skin examination. Multiple skin-coloured to red nodules are noted overlying the extensor surface of the distal interphalangeal joints of her right index and middle fingers as well as the proximal interphalangeal joint of her left index finger (Figure). The patient recalls these nodules being present for at least five years. They are intermittently painful but not itchy and do not ulcerate or develop blistering change. She has no similar skin changes elsewhere.
The patient’s medical history includes hypertension, hyperlipidaemia, asthma, osteoarthritis and gastro-oesophageal reflux disease. She reports a diet high in red meat and seafood and she drinks between three and four glasses of wine on most days of the week.
Differential diagnoses
Differential diagnoses to consider in a patient with multiple nodules on the dorsal surface of the hands include the following.
- Rheumatoid nodules. These nodules are the most common cutaneous and extra-articular manifestation of rheumatoid arthritis, a chronic autoimmune disease characterised by synovitis that leads to progressive joint destruction.1 Rheumatoid nodules present as mostly asymptomatic skin-coloured nodules with a predominance for extensor surfaces and skin areas prone to repetitive trauma, such as the forearms, fingers and metacarpophalangeal joints. Rheumatoid nodules are seen in up to 25% of patients with rheumatoid arthritis, and occurrence correlates strongly with seropositivity to rheumatoid factor antibodies; the nodules may precede onset of arthritic joint disease in 10% of cases.2 Biopsy of a rheumatoid nodule demonstrates a spectrum of features that relate to the stage of the nodule, ranging from an area of granulation tissue with adjacent angiogenesis, mononuclear infiltrate and fibroblasts (early), to a large focus of necrobiosis with accompanying fibrinoid deposition and lymphocytic infiltrate (late).2
- Heberden and Bouchard nodes. These nodes are a feature of osteoarthritis, the most common joint disease that affects between 10 and 20% of adults over the age of 60 years worldwide.3 These skin-coloured bony extensions are distinguished by location, arising from either proximal interphalangeal joints (Bouchard nodes) or distal interphalangeal joints (Heberden nodes).4 They are usually painless and can affect multiple digits. Imaging assessment of the nodes, such as x-ray, ultrasound or MRI, demonstrates characteristic degenerative joint changes such as osteophyte formation. Biopsy is rarely indicated to confirm the diagnosis.
- Subcutaneous granuloma annulare. Granuloma annulare is an idiopathic granulomatous disease that can be triggered by infection, trauma, arthropod bites and sun exposure.5 The subcutaneous variant is rare, and mostly affects children and adolescents.6 The lesions of subcutaneous granuloma annulare present as nontender nodules with normal overlying skin that involve the extensor surface of the hands and lower limbs, as well as the head and gluteal skin.6 Biopsy is diagnostic and demonstrates necrobiotic foci with accompanying peripheral palisading granulomas involving the deep dermis and subcutaneous tissue.5,6
- Multicentric reticulohistiocytosis. This very rare idiopathic histiocytic condition is associated with arthropathy. Risk factors include caucasian ethnicity and female gender; peak onset is in the fourth decade of life but the disease can present at any age.7 Associated diseases include hyperlipidaemia and mycobacterial infections, as well as solid-organ and haematological malignancies.7 The cutaneous changes in multicentric reticulohistiocytosis include the development of multiple skin-coloured to dark brown papules and nodules that favour the ‘H’ area of the face, trunk and periarticular skin of the hands and upper limbs.8 Unlike the nodules of subcutaneous granuloma annulare and the Heberden/Bouchard nodes of osteoarthritis, the skin lesions of multicentric reticulohistiocytosis cause significant pain and pruritus. Periungual papules and nodules give a characteristic ‘coral bead’ appearance; other skin manifestations of the disease include xanthelasma (yellow papules) and erythematous macules affecting sun-exposed sites.7 There may be associated arthritis as well as constitutional symptoms, such as unintentional weight loss and fevers. Most patients with multicentric reticulohistiocytosis (66%) develop arthritis as the first sign of disease with papulonodular eruption developing later, but 20% of patients develop skin changes first.7 Biopsy demonstrates a histiocytic infiltrate involving the dermis with multinucleated giant cells and accompanying lymphocytes.
- Gouty tophi. This is the correct diagnosis. Gouty tophi are the most common cutaneous manifestation of gout, a chronic metabolic disease characterised by prolonged serum hyperuricaemia that results in deposition of urate crystals in the synovium of joints that precipitate an inflammatory state.9,10 Risk factors for the development of gout include increasing age, male sex, obesity and a diet high in purine-rich foods (e.g. seafood, meat), fructose and alcohol.10 Chronic tophaceous gout has an insidious onset (over years) and can develop in the absence of acute gout attacks, although patients may recall painful polyarthritis coinciding with the development of gouty tophi. Deposition of urate crystals in the subcutaneous tissues results in the development of gouty tophi, which are firm subcutaneous nodules with a predilection for the joints of the hands, elbows and toes.9 Biopsy is not required for diagnosis but, if performed, demonstrates well-demarcated dermal nodular aggregates containing amorphous material with a perimeter of histiocytes in a palisading configuration. Polariscopic interrogation of these amorphous deposits shows negatively birefringent urate crystals.11
Management
The management of chronic tophaceous gout includes symptomatic relief for acute gout as well as urate-lowering therapy (ULT) to prevent further development of gouty tophi and systemic complications for serum hyperuricaemia.10 Liaising with the patient’s primary care physician is important to ensure monitoring of uric acid levels to titrate ULT as well as monitoring of renal function because of the known complication of gout nephropathy. In addition, monitoring of serum uric acid is important in patients with tophaceous gout because of their increased risk of cardiovascular mortality if the level is not corrected with ULT.12
A potential role for surgical intervention has been demonstrated where significant morbidity and disability result from gouty tophi and their destructive effects on joints.13
Outcome
In this patient, x-rays as well as a serum uric acid level measurement were performed, which confirmed destructive joint changes and hyperuricaemia indicative of chronic tophaceous gout. A skin biopsy was not performed. The patient’s pain subsided with regular oral ibuprofen 400 mg three times daily, and she then commenced ULT with allopurinol. She was counselled on the importance of lifestyle factors to prevent exacerbations of hyperuricaemia, including a diet low in fructose, purine and alcohol. MT
COMPETING INTERESTS: None.
